Posture influences how you move, the level of comfort you experience during daily activities, and how your body responds to physical effort. At Centrokinetic, digital postural analysis helps us understand these relationships objectively and build treatment plans aligned with your real goals. Below, we explain how we use the collected data to make practical therapeutic decisions that are easy to follow and adjust over time.
The purpose of our guide is clear: to show how digital postural analysis supports goal setting, reproduction of functional outcomes, and progress monitoring.
What is digital postural analysis?
Digital postural analysis is a computerized evaluation of body alignment. Modern systems use cameras and dedicated software to measure the position of the spine, pelvis, and main body segments. The assessment may include static posture and certain controlled movements to observe loading patterns and stability.
Unlike traditional visual observation, this method provides measurable data that can be compared over time. At Centrokinetic, we use this analysis as an integrated working tool within the therapeutic process. Technical details about the method and equipment can be found on the dedicated 3D Spine postural analysis page.
How do we integrate digital postural analysis into the treatment plan?

The process follows a clear structure, with defined steps tailored to each patient. The sequence remains the same, but the content is adapted according to individual needs.
1. Defining goals together with the patient
Everything starts with a discussion. We clarify what is bothering you, which activities you want to perform more easily, and what expectations you have from therapy. For some patients, the goal means reducing pain while walking. For others, it means returning to training or improving tolerance for sitting.
These goals guide the interpretation of the data. Without them, numbers have no practical value.
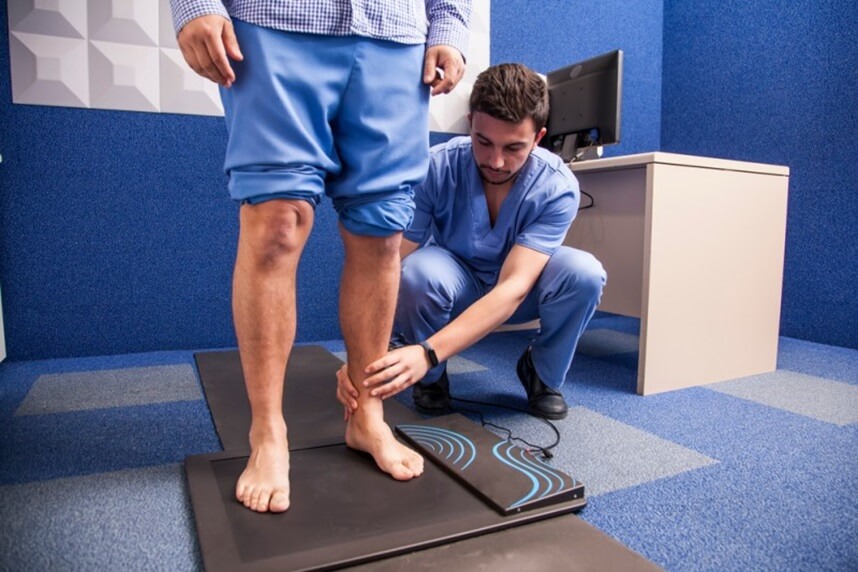
2. Data collection through digital postural analysis
We perform the assessment under standardized conditions. The patient adopts predefined positions, and the system records alignment and weight distribution through discreet sensors placed on key reference points. The data are processed by software that generates clear and easy-to-understand reports.
Measurements include:
- head and shoulder position;
- spinal alignment;
- pelvic position;
- symmetry of weight-bearing on the lower limbs.
3. Interpretation of results and identification of deviations
This is where clinical experience becomes essential. Postural deviations represent measured differences compared to what is considered functional alignment. They do not represent a diagnosis on their own. We correlate digital data with the physical examination, mobility tests, and medical history.
For example, pelvic rotation may have different relevance in a sedentary person compared to an athlete. In most cases, context makes the difference.
4. Correlating results with interventions in the treatment plan
Based on interpretation, we select interventions that directly address the identified issues. If we observe impaired movement control, we introduce specific stabilization and coordination exercises integrated into physiotherapy sessions. In certain situations, we associate physiotherapy procedures to support tissue adaptation.
5. Implementation of the personalized plan
The plan is applied progressively. Each session has clear objectives, and exercises are adapted according to the patient’s response. We monitor movement quality and the ability to transfer progress into daily activities, not just correct execution in the clinic.
6. Monitoring progress through periodic reassessments
Postural reassessment helps us verify whether the chosen direction remains appropriate. We compare the initial data with those obtained after several weeks and adjust the plan if needed. This approach is especially useful in managing low back pain, where progress occurs gradually.
7. Patient communication and education
We explain results in accessible language. Patients understand what each deviation means and why certain exercises are prioritized. Postural education supports maintaining results, especially in posture correction processes.
How do we use digital data in daily practice at Centrokinetic?
| Process stage | What we assess | How it influences treatment |
|---|---|---|
| Initial assessment | Alignment and stability | We establish priorities |
| Active sessions | Movement control | We adjust exercises |
| Reassessment | Measurement evolution | We optimize the plan |
Benefits, limitations, and risks to avoid
Digital postural analysis provides clarity and consistency, but it has limitations. It does not replace imaging investigations and does not establish a medical diagnosis.
Advantages include:
- use of validated equipment;
- data interpretation by trained professionals;
- respect for confidentiality and informed consent;
- avoidance of inappropriate treatment decisions.
Frequently asked questions
What is a postural deviation?
A postural deviation represents a measured difference from functional alignment, always interpreted within a clinical context.
Is digital postural analysis painful?
No. The assessment is non-invasive, 100% radiation-free, and does not cause discomfort.
How often is postural reassessment recommended?
The interval depends on the objectives and the treatment plan. In practice, reassessment is performed after several weeks or months.
Can this evaluation also be used preventively?
Yes. For many people without pain, the analysis helps identify loading patterns that may become problematic over time.
For stable results, integrate digital postural analysis into a comprehensive evaluation and treatment process. Discuss openly with your physician or physiotherapist and monitor your progress over time.
Disclaimer: This article is for informational purposes only and does not replace medical consultation. For interpretation, diagnosis, and personalized treatment plans, consult a physician or physiotherapist.
BUCHAREST TEAM
CLUJ NAPOCA TEAM
BRASOV TEAM
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT


















































































































































