See details
READ MORE
Recovery after high tibial osteotomy
Medical recovery after HTO is an important part of the healing process and a longer process compared to other knee interventions such as total or unicompartmental knee arthroplasty. The physiotherapist is the one who decides to implement this protocol in an appropriate treatment plan. The exercise waves can be adapted according to the equipment of the recovery clinic. This protocol must also be adapted to the patient and his preoperative deficits.Indications for high tibial osteotomy.
This surgery is indicated in the treatment of dislocated knee, with joint stiffness, in the case of arthritis in active middle-aged patients or in young patients who suffered a fracture in the growth cartilage as a child. The anatomical axis that crosses the knee allows a variation of 5-7 valgus. The total weight force transmitted through the knee is divided into 60% at the medial compartment and 40% at the lateral compartment. Additional ligament instability may increase the load on the medial compartment.The purpose of corrective osteotomy is often to relieve pain in the medial compartment and slow down the process of osteoarthritis by redistributing weight to the knee as close to normal as possible. Clinical indications for this procedure include varus deviation in orthostatism associated with:
- Gonarthrosis in the medial compartment and pain that limits activity
- Medial compartment gonarthrosis with ligament deficiency and clinical instability
- Gonarthrosis of the medial compartment with internal meniscus injury or joint cartilage injury
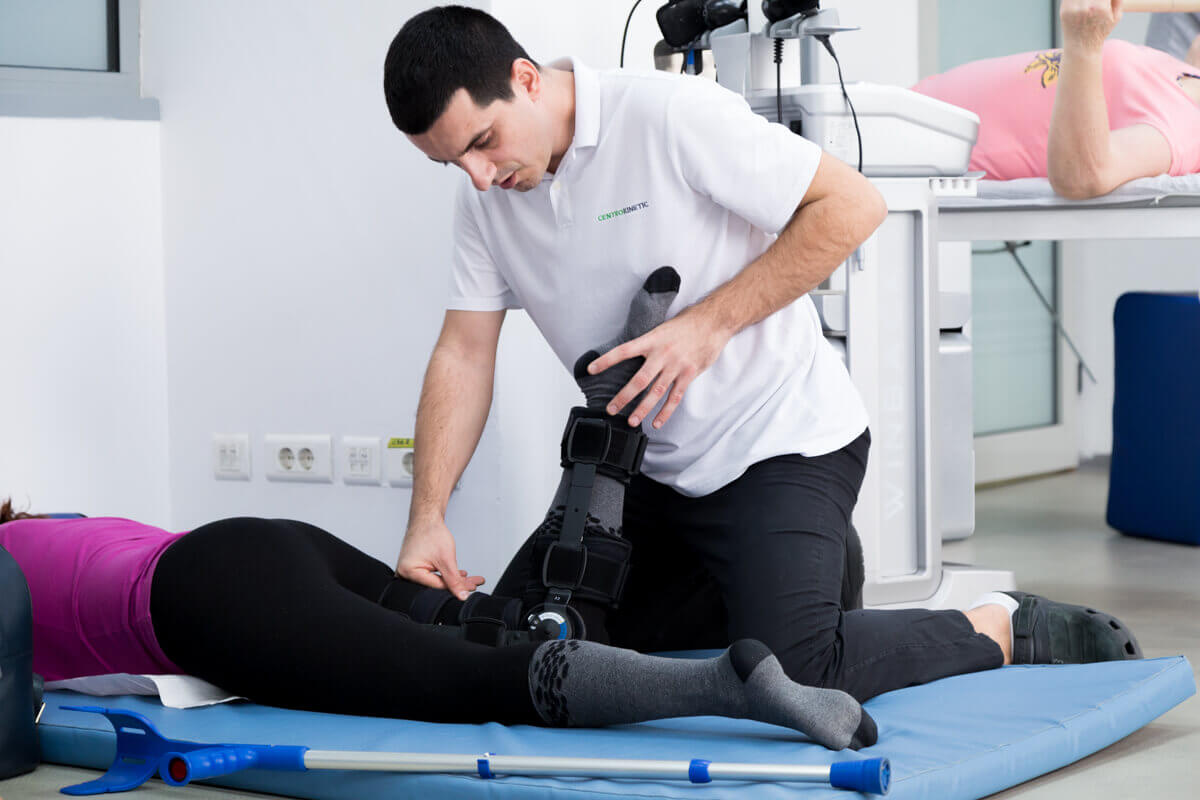
Patient education.
Postoperative indications include: walking with partial load (crutches or frame) with the hinge orthosis for six weeks. The permitted loading instructions are given by the surgeon and differ depending on several factors including the degree of correction that was required and the type of implant used. In the case of unstable osteotomies, or complications in terms of healing, patients are instructed to use crutches for a longer period, and full loading will be delayed.Resumption of activities/sports
Complete HTO healing, defined by the absence of pain and resumption of activities, including any exercise, can last up to 6 months or more. There are studies and reports on limb alignment, bone healing rate, time until full load walking, walking speed, knee joint dynamics, and subjective patient data on pain, functionality, and quality of life at 6, 12, 28, and 24 months postoperative.
Phase I: immediately postoperatively (0-2 weeks)
Objectives:
- re-education of the patient, use of crutches and loading within the limit indicated by the surgeon, orthosis is worn all the time, including at night; can be removed during physical therapy exercises.
- relieving pain and edema
- flexion up to 90 and full extension up to 2 weeks
- maintaining the calf and thigh muscles, working the quadriceps and gluteal muscles.
Exercises indicated
Flexibility:- Flexion/extension of the knee with the heel sliding on a flat surface (or on rollers)

- Assisted active flexion (with a towel) of the knee, sitting
- Stretching the leg (with a towel or elastic), with the knee in extension (gastrocnemius), or flexed (sole)
.jpg)
Strengthening the muscles
- Quadriceps - isometric contractions
- Gluteal - contractions in supine or orthostatism, flexion/extension, and adduction/abduction of the hip in orthostatism
- Shins - ankle flexion/extension
Phase II: muscle-strengthening without load (2-6 weeks)
Objectives:
- Use of crutches and limited loading indicated by the surgeon for 6 weeks post-op; the degree of activity is dictated by the installation of local pain and edema
- Movement range: >120 flexion and complete extension up to 6 weeks
Exercises indicated
Scope of movements:- Knee extension flexion exercises continue (with or without rollers)

Extension
- Passive extension of the knee from a sitting position, with a roll under the heel.
- In a prone position with the knees at the edge of the bed, passive extension.
- In supine position with legs raised on the wall - flexion of the knees with the heel on the wall, assisted by gravitational force.
- In a supine position, knee flexion on a medicine ball.
- In a prone position, knee flexion (assisted).
- The medical bicycle - with the seat up, rotating forward/backward, then complete rotations - lowers the seat according to tolerance.
Cvadriceps
- Isomeric contractions in a sitting position, supine position, orthostatism
- Leg extension with a roll below the knee
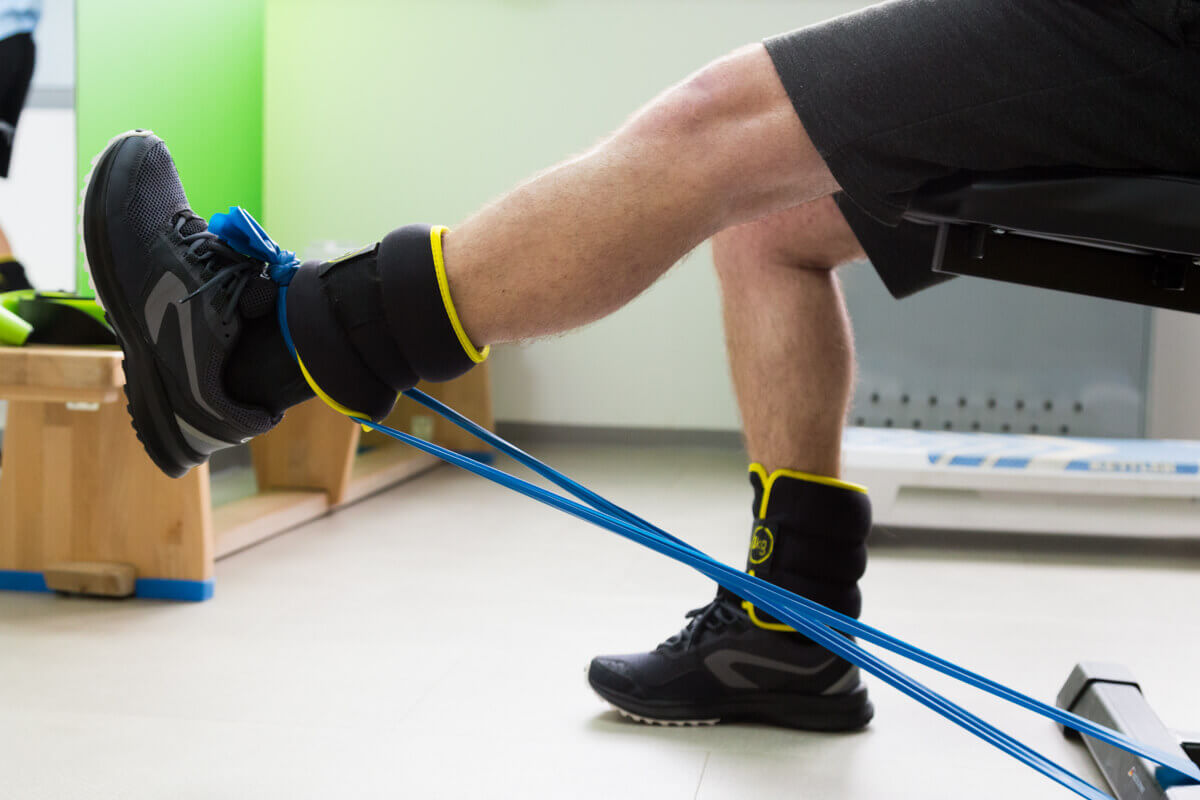
Hip / gluteus / posterior thigh
- In a supine position, lift the leg with the knee extended
- Flexion/extension, and adduction/abduction of the thigh, in orthostatism - pulleys or elastic bands can be inserted
- Knee flexion in a prone position
- In supine position - lifting the pelvis (with the base on 2 legs, then on 1 leg)
- In supine position - lifting the pelvis on the gym ball
Phase III: progressive weight gain and muscle-strengthening (6-12 weeks)
Objectives:
- Walking with load according to the doctor's instructions: walking with progressive load
- The orthosis is worn according to the doctor's instructions
- Monitoring and normalizing the walking position
- Complete range of knee movement and painless
- Initiation of cardiovascular exercises
Indicated exercises:
Scope of movements:- Mobilize the tibiofemoral joint, if necessary, for a full range of motion
- Medicinal bicycle
- Quadriceps extension in lateral decubitus, ventral decubitus or orthostatism
- Stretching exercises for gastrocnemius and solarium with full or partial load
- Advance from 2 crutches to one crutch, then full load, maintaining normal posture while walking
- Balance sideways and forward on the operated leg, using a scale
Quadriceps:
- Wall flexions starting at 30 and continuing at 60-90
- Change from sitting upwards, with the seat as high as possible and lowering according to tolerance
- Low weight press with both feet
- Walking with elastic bands: front, back, and side
- Stepper 5-10 cm high, side and front
- Strengthening the hips with weight advancement / elastic band resistance
- Leg flexion in a supine position with weights
- Lying on your back, with your feet on the gym ball - lift your pelvis and bend your knees
- Leg extension from sitting position with weights
- Walking on peaks
Cardiovascular exercises - cycling.

Phase IV (resumption of sports activities)
Objectives:
- Continuation and advancement in difficulty of exercises for the gluteal, quadriceps and posterior muscles of the thigh
- Continuation of cardiovascular exercises
- Continuation of balance exercises
- Resumption of sports training
Quadriceps:
- Lifting from a sitting position, with the progressive decrease of the seat height
- Step-up on the side and in front 10-15-20cm high

Buttocks and posterior thigh:
- Abduction and extension of the hip
- Leg flexion in a prone position with weights
- Progressive increase in weights and exercise intensity
- Balance in one leg on the irregular surface


MAKE AN APPOINTMENT
CONTACT US
SUCCESSFUL RECOVERY STORIES
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT

























































































































































