Disc herniation: types, why it occurs and how we treat it without surgery
- What is a herniated disc?
- Types of disc herniation
- Causes of disc herniation
- Symptoms of a herniated disc
- How to treat disc herniation
- How to prevent disc herniation
Dr. Bogdan Rotaru, primary neurologist, who specialized in electromyography, wrote this article.
Given that the major risk factors are sedentary lifestyle, smoking, and obesity, a herniated disc is a disease increasingly present in the lives of people in the 21st century. We have all experienced, at least once, an episode of back pain, so many people do not even know that they suffer from this condition in the early stages, attributing the pain to an uncomfortable position or a bad day.
The incidence of this pathology therefore becomes a real problem for modern society, which led us to shed light on this controversial topic. The pursuit of instant solutions with minimal effort has pushed discussions about surgery to the top of the priority list of patients diagnosed with a herniated disc.
Experience has shown us, however, that the herniated disc heals better when we don't undergo surgery but follows a series of physiotherapy procedures recommended by the specialist. Thus, we eliminate the risk of undergoing another surgery, just a few months after the first.
Centrokinetic provides you with a department dedicated to spinal disorders, especially herniated discs.
We will tell you further what are our arguments according to which the herniated disc surgery should be your last option, not before talking about what this condition means, what are the causes and how it manifests, so you can weigh the existing treatment methods before you follow the best option for you.What is a herniated disc?
In order to talk about a herniated disc as a neurological condition, which comprises the movement of vertebral discs of the spine, we must first understand how the spine works and what it is made of. The spine comprises a series of bones called vertebrae linked by an intervertebral disc which consists of a fibrous membrane, resistant on the outside and soft and elastic on the inside.This intervertebral disc, if healthy, works as a shock absorber that, besides keeping the spine straight, healthy, in a correct posture, also protects it from shocks caused by running fast or lifting weights. When the discs deteriorate because of aging or injury, the fibrous membrane ruptures, the overall pressure on the central area increases, and thus the disc herniation occurs.
Types of disc herniation
Although it can occur at any level of the spine, the most common forms of hernia are those in the lumbar (lower back) and cervical (neck) - areas of the body that we use mainly in everyday life, when we bend down to tie laces or when we sleep on our side. Depending on the affected area, the pain manifests itself differently.Lumbar disc herniation
If the movement of the intervertebral disc occurs at the lumbar level, the condition is called a lumbar disc herniation. The symptoms of lumbar disc herniation manifest as pain in the buttocks, thighs, and below the knees. The most affected nerves are the sciatic (longest nerve in the body) and the femoral nerve. Tingling, numbness, and tenderness in the affected limbs and areas may accompany the pain.Cervical disc herniation
If the herniated disc is located in the upper part of the spine, the condition is called a cervical disc herniation, and the sensation of pain will appear in the shoulders and arms. Such pain increases progressively in intensity and may be accompanied by tingling or numbness.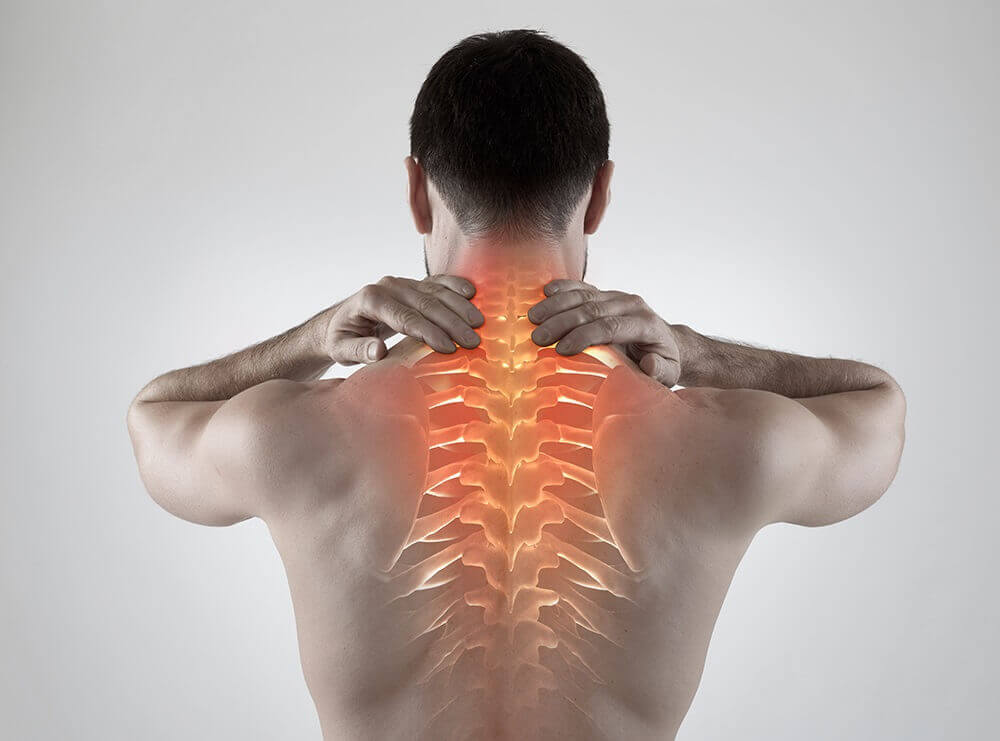
Causes of disc herniation
Specialists believe that a herniated disc has an important genetic component, especially in patients with a lumbar hernia, but most of the risk factors that favor the appearance of a herniated disc are closely related to the fast-forward lifestyle we all know very well:- smoking
- predisposition to sedentariness
- prolonged sitting
- Exaggerated physical exertion after long rest
- lifting weights the wrong way
- aging
- spinal injuries
Symptoms of a herniated disc
The symptoms differ from patient to patient but also depending on where the hernia is. The pain may increase gradually, radiating along the nerve fibers, from moderate to very intense. If hernias are not diagnosed early, it can get worse quickly. Many people postpone seeing a doctor because the symptoms are nonspecific. In other cases, patients have a herniated disc, but no symptoms.In the case of cervical hernias, the patient has muscular asthenia in the upper limbs, intense pain in the shoulders and scapulae, pain in the neck region, inability to turn his head or make sudden movements, radiated pain in the shoulder, arm, forearm and less often at the level of the palm, fingers, spasm of the upper vertebral muscles, sharp pain when laughing, coughing, sneezing.
In herniated discs, the pain is continuous, not pulsating.
The diagnosis of disc herniation is made after clinical examination and imaging, such as radiography, MRI, computed tomography, and myelography.
Symptoms of lumbar hernia
In the case of lumbar hernias, the patient feels pain in the buttocks and thigh, pain that can radiate to the calf and even the foot. Among the nerves involved, it is most often the sciatic nerve, determining the classic clinical aspect of sciatica, but the femoral nerve can also be affected. Tingling, numbness, sensitivity disorders may accompany these pains.The symptoms of a lumbar disc herniation have a sudden onset.
The acute period designates the stage of evolution of the disease in which the pains are intense and does not calm down no matter what position we adopt, which creates a major discomfort. In the subacute period, however, the pain in the sitting position disappears, so that the patient can move more easily, can sit on a chair for a certain period, and can move.
Symptoms of lumbar disc herniation with an insidious onset
The chronic period allows the patient to mobilize his spine, these mobilizations triggering moderate, bearable pain. In orthostatic position and gait, pain occurs after a long time, and contractions of the lumbar paravertebral muscles may persist.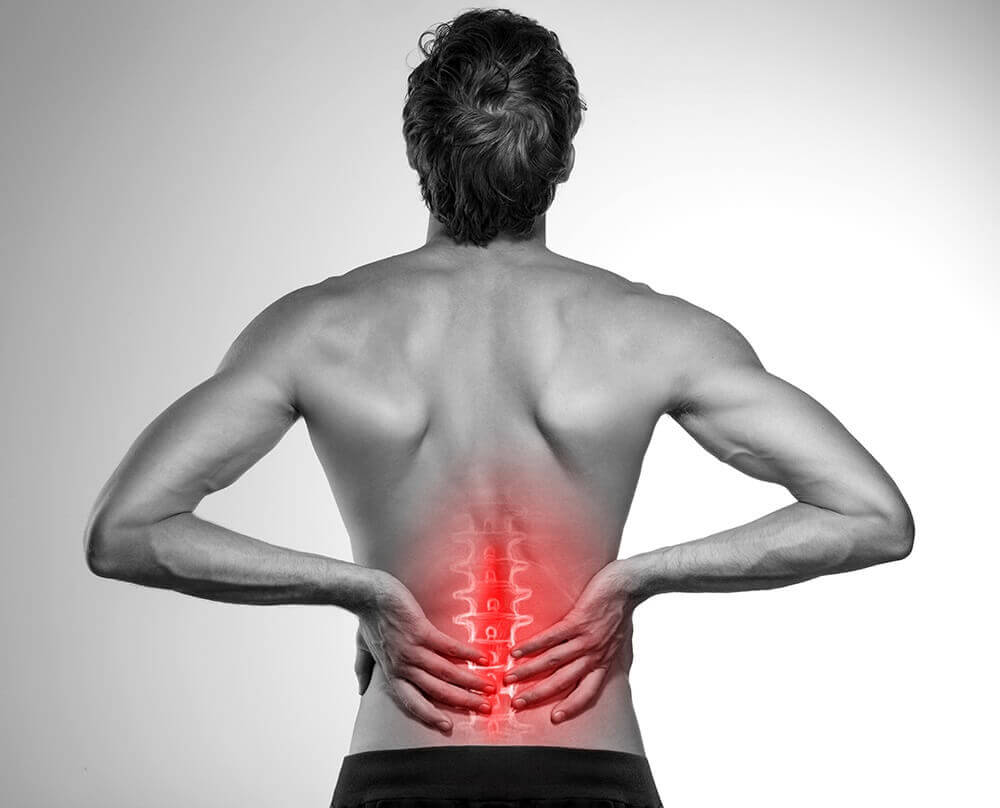
Stages of lumbar hernia
Phase I: disc instability phaseThere is intermittent chronic low back pain of postural type. It often disappears when the physical effort ceases or when resting. It can reappear under various conditions of effort.
Symptoms:
- pain in the lumbosacral area;
- the pain radiates to the limb on the side of the disease;
- the pain has mechanical causes and calms down at rest;
Symptoms:
- the pain starts suddenly;
- unilateral/bilateral lumbosacral pain;
- the pain has mechanical causes;
- without irradiation or with irradiation up to the knees;
This phase of the herniated disc has three stages of damage, namely:
- Irritant stage - the herniated disc reaches the nerve root which it compresses without compromising it.
- Compressive stage - the herniated material reaches the nerve root, which, although it does not damage it, compresses it.
- Interruption stage - in this stage, besides the signs and symptoms present at stages 1 and 2, signs are resulting from the sectioning of some axons in the root or the entire root by conflict with the herniated disc. It is found that the patient cannot stand on his toes in case of paralysis of the S1 root or that he cannot stand on his heels in case of L5 roots palsy.
Dysarthrosis and inter-apophyseal osteoarthritis appear (after 40 years). As we age, the nucleus pulposus suffers from dehydration, which favors the degenerative process of the intervertebral disc. The fibrous ring that covers the disc undergoes major changes due to the mechanical wear to which the spine is subjected.
How to treat disc herniation
If you have been diagnosed with disc herniation and still the symptoms are not unbearable, do not neglect the treatment just because you feel good at the moment. Its postponement leads to complications such as chronic pain, impaired mobility, or permanent injuries.The purpose of disc herniation treatment is to relieve pain and stop the progression of the condition.
Can a herniated disc be treated without surgery?
Yes, the herniated disc should be treated primarily by alternative methods such as physiotherapy and physical therapy, surgery remaining a last resort. The treatment of disc herniation includes personalized measures - physical therapy, physiotherapy, cortisone injections, avoidance of harmful efforts or positions, anti-inflammatory and/or muscle relaxants (relaxation of the paravertebral muscles), and, in the last case, surgery.Complementary treatment for disc herniation includes acupuncture, therapeutic massage, yoga.

Disc herniation without surgery
Given that surgery should be recommended only in 10% of cases, which are severe, where the pain persists even after 5-6 weeks of alternative treatment, non-surgical treatment is a pressing requirement and it should always be followed first. We'll tell you below which are the most popular and beneficial therapies for healing a herniated disc without surgery.Physical therapy in the treatment of disc herniation
Decreasing the pressure exerted on the disc and the affected nerve is one of the major objectives in the treatment of disc herniation. Therefore, physiotherapists recommend exercise with a specific role in this condition. Their purpose is to tone the back muscles. Thus, a correct back position will be obtained. The spine is stabilized in the long run, and the pain is reduced, the condition being effectively treated by physical therapy.
Physiotherapy in the treatment of disc herniation
Physiotherapy treatment in disc herniation is beneficial in relieving pain and involves electrotherapy, hydrotherapy, balneotherapy. The major effects of this form of treatment are anti-inflammatory, decontracting, and hyperemic. Because there are many forms of electrotherapy in the treatment of disc herniation - interferential currents, galvanic current, etc. - the treatment may be shorter due to the combination of procedures.
Massage, adjuvant treatment in disc herniation
Massage relaxes muscles and stimulates the secretion of intra-articular synovial fluid - a fluid that feeds the soft structures inside the joints, including the intravertebral disc - being beneficial in muscle contractions. Thus, it calms the pain and improves the local blood circulation. Massage is a very popular procedure for patients with a herniated disc due to its strong and fast analgesic effect.
In disc herniations, elongations are extremely effective and non-invasive. It is a three-dimensional decompression of the vertebrae. Technological traction executed in perfect parameters will correctly reposition your vertebrae.
Following this procedure, the intervertebral discs are unlocked, which favors the healing environment. Everything takes place safely and with no pain. Accompanied by physiotherapy, the effects are felt right after the first session: reduction of the intensity of pain and inflammation, relaxation of the muscles, and even an increase in height of one or two centimeters.

Kinesiotaping in disc herniation
It is an adhesive bandaging technique, designed to facilitate the healing process. The kinesiological tape is made of cotton and has acrylic adhesive. Its elasticity is often similar to that of human skin. The properties of the adhesive are activated by body heat, and the tape is water-resistant, being able to be worn even for several days and thus speeding up the recovery process. The effects of the kinesiological band are aiming at pain relief, the improvement of the muscular functions, the direction of the movement, the position of the joints, and the lymphatic drainage. All these services are available at Centrokinetic. For a correct diagnosis and a well-structured treatment plan, with real objectives, you can schedule a consultation.
Disc herniation surgery
The operation comprises the surgical removal of the fragments of the disc or even of the entire herniated disc that presses on the nerve roots, but often there are risks associated with surgery.The biggest problem with surgery, in this case, is that the herniated disc may appear completely removed, without this really happening, leaving behind small particles on the vertebrae.
Over time, the lack of the intervertebral disc can cause additional pain, because the space between the vertebrae remains free and the other discs can move. In most cases, this evolution of the problem comes with the recommendation to perform a new surgery.

How to prevent disc herniation
To prevent the onset of disc herniation symptoms, we must first eliminate the factors that cause it. Although we have no way of intervening on genetic inheritance, we can contribute to all the other causes listed above. • Quitting smoking
An important risk factor for disc herniation is smoking. It can interfere with the correct oxygenation of the spine and implicitly of the disc. Thus, dehydration and disc degeneration can occur, which can cause disc herniation over time.
• Weight loss
Excess weight - from overweight to morbid obesity - is a cause of disc herniation. By maintaining an optimal weight, we reduce the mechanical forces that act on the body and thus prevent the degradation of the spine and lower limb joints.
• Properly dosed physical effort
Disc herniation can also occur because of an overload of the body in an intense physical effort, so we recommend avoiding effort over the known capacity of our body. In the case of practicing different sports, we recommend performing appropriate exercises to warm up the required joints.
• Correct posture
To prevent the appearance of lumbar disc herniation we must avoid overloading the lumbar spine by lifting weights in incorrect positions (with the back flexed or in hyperextension), positions that stress to the maximum the fibrous ring. The patient feels a violent pain that immobilizes him and that no longer allows him to straighten his spine, flex, rotate, or extend it.
In current activities, body posture has great importance in preventing the appearance of lumbar hernia, for example: tying the laces should not be done by hyperflexion of the trunk, but with the lower limbs flexed or sitting.
In the long run, it has been shown that better results are obtained for the patient by replacing the surgery with a personalized recovery program through physiotherapy and physical therapy. Instead of removing the herniated disc, this method comprises exercises that gradually push the disc into its original position. To return to pre-diagnosis health, the patient must follow complex physical therapy programs, under the guidance of an overspecialized medical team.
At Centrokinetic, the best doctors and therapists are at your disposal for any joint or musculoskeletal disorder, from initial consultation and complete investigations in the clinic, to treatment and complete medical recovery in spinal, traumatic or post-surgical conditions.
- Orthopedics , a department composed of an extremely experienced team of orthopedic doctors, led by Dr. Andrei Ioan Bogdan, primary care physician in orthopedics-traumatology, with surgical activity at Medlife Orthopedic Hospital, specialized in sports traumatology and ankle and foot surgery.
- Pediatric orthopedics , where children's sports conditions are treated (ligament and meniscus injuries), spinal deformities (scoliosis, kyphosis, hyperlordosis) and those of the feet (hallux valgus, hallux rigidus, equine larynx, flat valgus, hollow foot).
- Neurology , which has an ultra-performing department, where consultations, electroencephalograms (EEG) and electromyography (EMG) are performed.
- Medical recovery for adults and children , department specialized in the recovery of performance athletes, in spinal disorders, in the recovery of children with neurological and traumatic diseases. Our experience is extremely rich, treating over 5000 performance athletes.
- Medical imaging , the clinic being equipped with ultrasound and MRI, high-performance devices dedicated to musculoskeletal disorders, and complemented by an experienced team of radiologists: Dr. Sorin Ghiea and Dr. Cosmin Pantu, specialized in musculoskeletal imaging.

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT

















































































































































