See details
READ MORE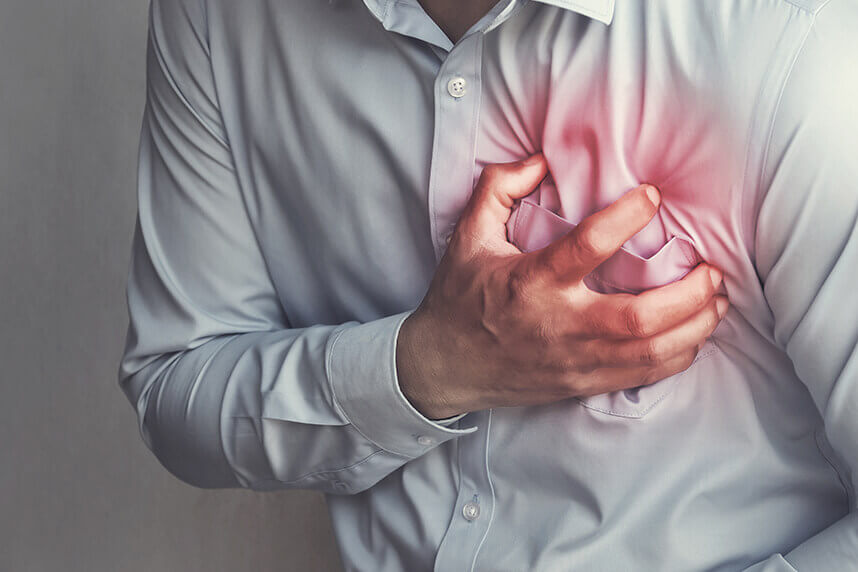
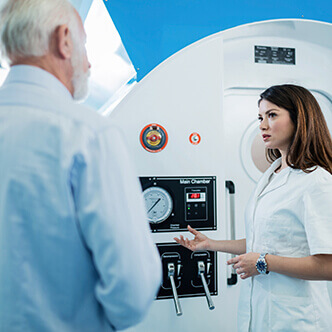
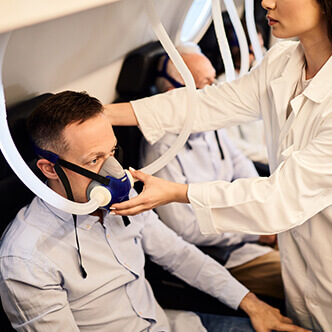
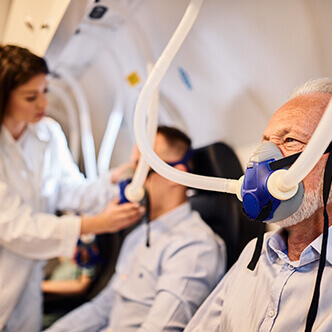
Discover the hyperbaric medicine center opened in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest, with multiple medical and anti-aging uses. The Baroks chamber has 5 seats, and operates at a constant pressure of 2.5 atmospheres, being fully automated and having protocols for each condition, and can be used individually for each patient.
Hyperbaric oxygen therapy - benefits
Patients who use the clinic's hyperbaric therapy services benefit from:
- The only medically accredited hyperbaric therapy chamber in Bucharest, which operates at 2.5 atmospheres (those for aesthetic use go to 1 atmosphere and have no medical benefits).
- A safe medical procedure, without irradiation, without pain, without other side effects.
- The specialized medical team consists of recovery doctors, orthopedists, rheumatologists, neurologists, and neurosurgeons, meaning a multidisciplinary team specialized in all diseases that can be treated with hyperbaric therapy.
- Premium conditions at a fair price. Our clinic is recognized for the conditions offered and for the care of each patient. But we do not need to pay exorbitant prices to have access to quality medical services. At Centrokinetic you can find an affordable and fair price. But note that we do not have a contract with the National Health Insurance House (we do not offer state reimbursed services)
Centrokinetic is keeping contact with prestigious clinics and universities in Belgium, the Netherlands, France, and Greece to constantly update treatments to provide patients with the best medical solutions.
 | .jpg) |
The extra oxygen protects the heart against acute myocardial infarction
The present study aimed to determine an optimal oxygenation protocol that can be applied clinically for the treatment of acute MI. Using EPR oximetry, we studied the effect of exposure to the supplemental oxygen cycle (OxCy) administered by inhalation of 100% oxygen for short periods (15–90 min), daily, for 5 days, in rats with acute MI.
Myocardial oxygen pressure (pO2), cardiac function, and pro-survival / apoptotic signaling molecules were used as markers of treatment outcome. OxCy has led to a significant reduction in the size of the heart attack and improved heart function. It was found that an optimal condition of 30 min OxCy with 95% oxygen + 5% CO 2 in normobaric conditions is effective for cardioprotection.
It is reasonable to assume that the administration of pure oxygen during and after a cardiac event to increase the delivery of oxygen to the blood in the affected heart tissue would reduce the size of the infarction and save the risky myocardial tissue. In turn, it is expected that this will lead to an ambiguity of functional recovery. In most circumstances, the provision of additional oxygen to patients with suspected MI by emergency responders is routine. Until recently, some recommendations included regular administration of oxygen for the treatment of MI. However, this position has changed, so that continuous oxygen treatment is recommended only in certain circumstances and not for uncomplicated cases of MI. This change in treatment protocol is likely to be due to known hemodynamic side effects associated with hyperoxygenation. Hyperoxygenation of patients with acute MI results in an increase in blood pressure and a reduction in cardiac output. These changes have been attributed to decreased heart rate and stroke volume and increased vascular resistance. Hyperoxygenation is also a strong stimulant of coronary circulation and vasoconstriction.
What are the effects of oxygen therapy on the body?
- Decreases inflammation
- Increases the body's oxygen saturation by 20-30%
- Increases the body's immunity
- Increases blood circulation and stimulates the formation of new capillaries
- Decreases toxins in the body
- Stimulates the production of new blood cells
- Increases healing rate
In addition to normobaric oxygen, hyperbaric oxygen (HBO) has also been investigated as a potential therapeutic measure for MI. A study by Cameron et al. reported that the hemodynamic effects of oxygen therapy in patients with MI at normal pressure (1 ATA) were improved after an increase to 2 ATA. In 1998, the "HOT MI" study attributed a higher left ventricular ejection fraction in the HBO-treated group to increased myocardial rescue compared to untreated subjects. In 1969, Ashfield and Gavey enrolled and evaluated 40 volunteers who were treated with HBOT continuously for 4 days in exposure periods of 2 h at 100% O 2 at 2 ATA, followed by 1 hour in the air chamber. at normobaric pressure.
.jpg)
The following report documents our attempt to investigate several problems, and the aim was to determine the optimal conditions for OxCy treatment (ambient pressure, % oxygen, exposure time, etc.) that are needed to prevent myocardial damage. Also, maximizing the benefits and quality of life for the subject. We found that, in general, HBOT led to a significant reduction in the size of the heart attack and an improvement in cardiac function.
Materials
Primary and secondary antibodies to Akt and pAkt were purchased from Cell Signaling Technology (Danvers, MA) and GE Healthcare (Little Chalfont, Buckinghamshire, UK). Polyvinylidene fluoride (PVDF) membrane and molecular weight markers were obtained from Bio-Rad (Hercules, CA). Antibodies specific for p53 and Bax were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Enhanced chemiluminescence (ECL) reagents were obtained from Amersham Pharmacy Biotech (GE Healthcare-Piscataway, NJ). The RIPA lysis buffer was obtained from Santa Cruz Biotechnologies. All other reagents, analytical grade or higher, were purchased from Sigma-Aldrich unless otherwise stated. LiNc-BuO microcrystals were synthesized as previously reported.
Experimental groups
After allowing 72 hours for post-surgical recovery, the experimental animals were treated with the help of the additional oxygen cycle (OxCy), by placing them in a custom-built room, every day, for 5 consecutive days under different treatment conditions. Acute myocardial infarction (MI) was induced by IR injury as described above. Animals with MI were treated with 4 different concentrations of additional oxygen (40, 70, 90, and 100%) for a period of 60, 30, or 15 minutes per day, administered under normobaric or hyperbaric pressure. Oxygen composition and administration times were chosen to cover a wide range to represent the most effective and easily applicable clinical conditions to arrive at an optimal treatment modality. The study was divided into a total of 10 groups with 5 major categories. Group 1: Control group that had neither MI nor was subjected to the oxygen cycle. Group 2: The MI group with animals were always kept in the air in the room without OxCy. Groups 3–5 received treatment for MI with 60 min of OxCy at normobaric pressure and were divided according to the additional oxygen concentration; 40% O2, 70% O2, or 100% O2. Groups 6-7 received treatment with 60 min of OxCy using 100% O2 in the hyperbaric chamber and were divided according to pressure 1.5 or 2 ATA. Groups 8-10 received treatment for MI with carbon (95% O 2 + 5% CO 2) at normobaric pressure and divided according to the duration of treatment: 15, 30, or 60 min. Each group contained 4-12 rats. Control group that had neither MI nor was subjected to the oxygen cycle.
Experimental setting
Myocardial infarction (MI) was induced by ischemia-reperfusion injury by temporary ligation of the LAD artery for 60 min. OxCy treatment was initiated after three days of rest. The study was divided into ten groups. Group 1 (control) did not have MI and did not receive OxCy treatment. Group 2 had MI, but these animals were kept in the air in the room without OxCy. Groups 3-5 were subjected to 60 minutes of OxCy using 40, 70, or 100% O 2 (N2-balanced), respectively, under normobaric conditions (NBO). Groups 6-7 received 60 min of OxCy under hyperbaric oxygen (HBO), using 100% O2 at 1.5 or 2 ATA. Groups 8–10 received OxCy using carbogen for 15, 30, or 60 min. Echocardiography and biomarker analysis were performed after five days of OxCy treatment.
Cardiac function was measured using M-mode echocardiography after five days of OxCy. The rats were anesthetized releasing 1.5-2% isoflurane in the air, and M-mode ultrasound images were obtained using a high-resolution Vevo 2100 ultrasound imaging system (VisualSonics; Toronto, ON, Canada).
After anesthesia followed by intubation, the animal's chest was reopened between the 3rd and 4th intercostal space, and the cavity was opened using a copper-based retractor wire. Using an internally produced moving syringe tip, a LiNc-BuO EPR oximetry probe was implanted in the left ventricular myocardial tissue. After making sure that the ventricular perforation did not take place, the rat was immediately transferred to a room built to order (diameter of 10 cm and length of 40 cm) with provisions for gas entry and exit. A resonator with a surface loop was inserted through a sealed port in the chamber and placed above the heart. An EPR unit for live oximetry (Magnettech, Berlin, Germany) was used for measurements. Basic EPR measurements were performed using room air (21% oxygen). When needed, hyper oxygen gas mixtures were passed through the chamber during the measurements. EPR spectra were taken as single 30-second scans. The instrument settings were: microwave frequency - 1.2 GHz (L band), incident microwave power - 4 mW; modulation amplitude - 180 mG, modulation frequency 100 kHz; receiver time constant - 0.2 s. The peak-to-peak width of the EPR spectrum was used to calculate pO2 using a standard calibration curve.
.jpg)
Analysis of molecular expression of proteins using Western Blotting
.jpg) | .jpg) |
Data analysis
The statistical significance of the results was assessed using unique tANOVA tests. Values were presented as mean ± standard deviation (SD). A p-value of less than 0.05 was considered significant.
Using EPR oximetry, we determined the effect of increasing inspired oxygen concentrations on myocardial pO2 in healthy (non-MI) rats. Myocardial PO2 increased from an initial value of about 14 mmHg to a level reaching even about 28 mmHg during exposure to carbogen (95% O 2/5% CO2). PO2 peaked at approximately 12 minutes after the start of carbogen administration and remained high above baseline (chamber air) after carbon dioxide depletion and re-exposure to chamber air. The results showed a concentration-dependent increase in maximum myocardial oxygenation, while carbohydrate exposure showed a significantly higher increase compared to all other groups. Interesting, exposure to 100% O2 showed a significant decrease in oxygenation peak compared to carbonation. Overall, the results indicated that rats' exposure to hyper oxygen increased myocardial pO2 during administration. We further determined the effect of the oxygen cycle on myocardial pO2 in rats at 1-week post-MI. The results showed significant differences in values between control, untreated MI, and OxCy-treated MI.
To determine the effect of the oxygen cycle on cardiac function, we used M-mode echocardiography on day 9 after IM induction. Significant decreases in ejection fraction and fractional shortening were observed in cases that did not receive oxygen therapy. Rats treated with all levels of hyperoxygenation, both at normobaric and hyperbaric pressures, showed variable levels of recovery of cardiac function depending on the level of oxygen inhaled. Rats subjected to hyperoxygenation (100% O2) at 1.5 or 2 ATA pressure, 1 h / day for 5 days, demonstrated remarkable recovery of cardiac function; however, the improvement at these hyperbaric levels was not significantly better than that at ambient pressure.
Postmortem analysis of cardiac tissue with TTC staining was consistent with echocardiographic data, with a substantial reduction in the infarction area in hearts with MI after oxygen therapy 95% 2/5% CO 2, 30 min/day. Acute MI, induced by surgical IR causes myofibrillary edema leading to myocardial dysfunction. To evaluate the effect of additional oxygenation on cardiac edema, we measured the weight of the whole heart, whole lung, right ventricle, and left ventricle with septum. The results showed a significant increase in weight, which was inhibited by oxygen cycle treatment with 95% O2 / 5% CO2 for 30 min/day.
To understand the basic signaling pathways involved in cardiac recovery after oxygenation, we analyzed the heart tissues using the Western blot test. We analyzed the following pro-survival and pro-apoptotic proteins, namely, Akt, eNOS (NOS3), pAkt, p53, and Bax, which were found to be critically involved in MI hearts subjected to OxCy. Blot images were quantified and data were normalized. Akt levels remained unchanged in all groups. Hearts with MI showed a significant reduction in the pro-survival protein pAkt compared to control hearts. Treatment with 100% oxygen at 1-2 ATA, as well as with 30 and 60 min of carbon significantly increased pAkt expression. Compared to hearts with MI, we found significantly elevated levels of eNOS pro-survival protein in hearts treated with 100% oxygen at pressures of 1, 1.5, and 2 ATA, and in hearts treated with carbogen for 30 or 60 min. There did not appear to be a tendency to increase p53 levels in the various treatment groups; however, it is relevant to note that hearts with infarction, as well as almost all treated hearts, displayed a higher overall expression of p53 after the oxygen cycle than control hearts.
The effectiveness of treatment with post-MI hyperoxygenation, whether in normobaric or hyperbaric conditions, has been a hotly debated topic, despite its widespread use in the last century. Two recently published reviews found a very limited number of randomized, controlled studies of oxygen in addition to normal air for patients with MI. In both reviews, the authors concluded that the studies did not show any benefit of oxygen therapy. These reviews were quoted in a recent editorial by Dr. C. Richard Conti, who states: After analyzing the literature, I could not find solid evidence that the use of supplemental oxygen (hyperbaric or normobaric) in an Uncomplicated acute myocardial infarction (AMI) is beneficial and there is some evidence that it could be harmful. Factors to consider when reviewing previous work are the timing and sequence of hyperoxygenation / HBO treatment and delivered oxygen concentration. In both the 1969 study by Ashfield and the study by Gavey and the 1976 study by Rawles, patients were treated within 24 hours of presenting MI. In another clinical study, patients were treated with normobaric hyperoxygenation following thrombolysis 6 hours after MI. Patients receiving oxygen treatment were given 100% masked oxygen for 24 hours. After mixing with the air in the chamber, it is estimated that the release of the face mask of 100% oxygen produces a FiO2 of 40%. Patients were treated within 24 hours of presenting MI. In another clinical study, patients were treated with normobaric hyperoxygenation following thrombolysis 6 hours after MI. Patients receiving oxygen treatment were given 100% masked oxygen for 24 hours.
In a study using rats, Santos et al. subjected the experimental animals to a single 1-hour period of HBO (100% O 2 at 2.5 ATA) immediately after coronary occlusion and observed a decrease in necrotic area and acute mortality. In the more recent "HOT MI" clinical trial, patients with acute MI underwent a single application of HBO immediately after thrombolysis. The results showed a 10% increase in the recovery fraction in the HBO group, rapid elimination of pain, and attenuation of creatine phosphokinase, although the results were not statistically significant.
In the current study and our previous work, hyperoxygenation or HBO treatment was started at 3 days post-MI in experimental rats. This recovery period was introduced to allow healing for pneumothorax created by the MI induction procedure. Tension pneumothorax is a contraindication to clinical HBO therapy. Non-HBO animals were also allowed this recovery period to avoid complicating the study, with different starting points for treatment. Our group also reported that restoring coronary perfusion following simulated IM in a rat produces hyperoxygenation in the affected region myocardial tissue for up to 24 hours and possibly longer.
Western blot studies have shown that hearts that are subjected to a combination of oxygen and carbon showed significantly higher expression of the pro-survival pAkt and eNOS proteins and lower expression of the pro-apoptotic Bax protein compared to other treatments. Interestingly, the p53 level was significantly higher in the carbogen groups (60 and 30 min) compared to the conventional treatment group. These results are consistent with our previous reports that used a similar experimental model.
Many previous animal or clinical studies have applied hyperoxygenation or HBO as a one-time intervention, or for 24 hours continuously. Compared to other hyperoxygenation or HBO protocols, such an approach is unique. The only previous work that used a periodic or cyclic approach was the Ashfield and Gavey study, in which treated patients were subjected to 2 hours of HBO with 100% oxygen, followed by 1 hour in air at normobaric pressure. This cycle was repeated continuously for an average of 4 days. As mentioned by Jain, repeated exposure to HBO at insufficient intervals to allow full recovery of lung toxicity can lead to cumulative effects. Following this warning, the cyclic process used in the current study, in which a single dose of 1 h was administered daily.
.jpg)
In the present study, HBO administered at 1.5 or 2 ATA did not provide significantly better results in terms of recovery of cardiac function compared with treatment with 100% oxygen administered at ambient pressure. For this reason, we conclude that hyperbaric conditions, although generally beneficial, are not entirely necessary or even practical for MI, in particular, considering a patient in a clinical setting that should be placed inside a room to synthesize such an environment. Carbogen, a mixture of 95% O2 and 5% CO2, improves the oxygenation of myocardial tissue to the greatest extent, and this increase was especially greater than when 100% oxygen was used. This is most likely due to two well-documented hemodynamic responses: Hyperoxygenation promotes vasoconstriction and CO2 is a powerful vasodilator. From these results, we claim that the vasodilating effect of CO2 exceeds the vasoconstrictive effect of hyperoxygenation. If the main goal of additional oxygen therapy as an adjunct to patients with MI is to increase oxygenation of myocardial tissue, then the use of hyperoxygenation should be considered given the patient's condition.
IN CASE YOU HAVEN'T ALREADY HEARD ABOUT US
Centrokinetic is the place where you will find clear answers and solutions for your motricity problems. The clinic is dedicated to osteoarticular diseases and is divided into the following specialized departments:
- Orthopedics , a department composed of an extremely experienced team of orthopedic doctors, led by Dr. Andrei Ioan Bogdan, primary care physician in orthopedics-traumatology, with surgical activity at Medlife Orthopedic Hospital, specialized in sports traumatology and ankle and foot surgery. .
- Pediatric orthopedics , where children's sports conditions are treated (ligament and meniscus injuries), spinal deformities (scoliosis, kyphosis, hyperlordosis) and those of the feet (hallux valgus, hallux rigidus, equine larynx, flat valgus, hollow foot).
- Neurology , which has an ultra-performing department, where consultations, electroencephalograms (EEG) and electromyography (EMG) are performed.
- Medical recovery for adults and children , department specialized in the recovery of performance athletes, in spinal disorders, in the recovery of children with neurological and traumatic diseases. Our experience is extremely rich, treating over 5000 performance athletes.
- Medical imaging , the clinic being equipped with ultrasound and MRI, high-performance devices dedicated to musculoskeletal disorders, and complemented by an experienced team of radiologists: Dr. Sorin Ghiea and Dr. Cosmin Pantu, specialized in musculoskeletal imaging.
Oxygen therapy in diving accidents
Diving accidents are accidents that can occur during diving, being specific to this activity, and are always an emergency. Learn the benefits of hyperbaric therapy and why it is useful in diving accidents.
READ MOREContraindications Of Hyperbaric Oxygen Therapy
Hyperbaric oxygen therapy has multiple medical and anti-aging uses. Like any medical treatment, hyperbaric oxygen therapy has certain contraindications. Find out here what are the contraindications for hyperbaric oxygen therapy.
READ MOREThe Effectiveness of Hyperbaric Oxygen Therapy in Reversing the Aging Process in Humans
Scientists in Israel say they can reverse the aging process. The key to this success seems to be hyperbaric oxygen therapy – breathing pure oxygen while sitting in a pressurized chamber for a certain amount of time. In this case, it's 90 minutes/session, with a frequency of 5 sessions per week, for 3 months.
READ MOREHyperbaric oxygen therapy in intestinal pneumatosis
Cystoid or cystic intestinal pneumatosis (intestinal emphysema) is a symptom that can occur in many gastrointestinal diseases. Hyperbaric oxygen therapy can be a successful treatment of cystoid intestinal pneumatosis and granulomatosis with polyangiitis.
READ MOREHyperbaric oxygen therapy in cell damage caused by radiation in gynecological cancers
Gynecological cancers treated with a combination of external beam radiation and brachytherapy, especially cervical and vaginal cancers, can result in the apex of the vagina receiving a high dose of radiation. Hyperbaric oxygen therapy has positive effects on the radiated tissues, especially the head, neck, anus, and rectum.
READ MOREHyperbaric oxygen therapy in post-radiotherapy CNS injury
Hyperbaric oxygen therapy involves the use of so-called levels of oxygen under pressure to increase the level of oxygen in the blood. The use of hyperbaric oxygen therapy involves oxygen treatment for soft tissue radionecrosis. Read this article and find out more.
READ MOREHyperbaric oxygenation vs normobaric oxygenation in CO poisoning
Prolonged CO exposure is responsible for more than half of fatal poisonings and is also one of the leading causes of poisoning in Western countries. We aimed to compare the effectiveness of therapy with hyperbaric oxygen (HBO) versus normobaric oxygen (NBO) in the setting of carbon monoxide poisoning (COP).
READ MOREHyperbaric oxygen therapy in diabetic foot
Hyperbaric oxygen therapy may be effective for Wagner's grade 3 and 4 diabetic foot ulcers and need to study the real problems with patients seeking treatment and demonstrates the need to study the real problems with patients seeking treatment. The results show that it is important to follow the treatment in order for the HBOT to be efficient.
READ MOREThe role of hyperbaric oxygen therapy in sports medicine
Hyperbaric oxygen is used in sports medicine to reduce hypoxia and edema and is also effective in treating stroke injuries and acute traumatic peripheral ischemia. When used clinically, hyperbaric oxygen should be considered as an adjuvant therapy used as early as possible after the diagnosis of the lesions.
READ MOREHyperbaric oxygen therapy in muscle injuries
Muscle stretches are the most common muscle injuries suffered during performance sports. Rapid recovery from muscle injury is crucial for elite athletes who regularly are exposed to training and increased competition. Hyperbaric oxygen therapy is a safe and effective method, being a non-invasive treatment
READ MOREHyperbaric oxygen therapy in sports injuries
Hyperbaric therapies are methods used to treat disease or injury using pressures higher than the local atmospheric pressure inside a hyperbaric chamber. The long-term effects are neovascularization (angiogenesis in hypoxic soft tissues), osteoneogenesis, and stimulation of collagen production by fibroblasts. This is beneficial for wound healing and recovery after irradiation.
READ MOREHyperbaric oxygen therapy in proctitis generated by radiation
Proctitis is the inflammation of the rectal mucosa causing pain, discharge, and other unusual symptoms. Pain can occur during bowel movements, it can be acute or chronic. Symptoms may vary, but the most common is tenesmus (the feeling of needing to go to the toilet), a sensation that persists even after using the toilet. This treatment should be offered to patients who fail to recover with conventional treatments for radiation-induced proctitis.
READ MOREHyperbaric oxygen therapy in refractory osteomyelitis
Osteomyelitis is an infection of the bone or marrow caused by bacteria or mycobacteria. Hyperbaric oxygen treatments can be considered an American Heart Association (AHA) Class II recommendation for the treatment of chronic, refractory osteomyelitis
READ MOREHyperbaric oxygen therapy in tinnitus
Hyperbaric oxygenation allows a controlled increase in oxygen pressure in the blood. This technique can be used in cases of tinnitus and sudden deafness, when certain changes in the inner ear and brain generate a lack of oxygen and, therefore, a limited intake of energy.
READ MOREHyperbaric oxygen therapy of ischemia and reperfusion injury
Hyperbaric oxygen therapy has been found to ameliorate the damaging effects of reperfusion by early modulation of inflammation, maintenance of metabolic function in downstream tissues, and reintroduction of oxidation scavengers.
READ MOREHyperbaric therapy in the treatment of second degree burns
HBOT has a beneficial effect on burn wound healing by reducing edema and ensuring there is adequate oxygen in microcirculation. It may speed up epithelialization and suppress unnecessary inflammation that could negatively affect normal wound healing. With further research, HBOT may become an adjuvant therapy to surgery.
READ MOREHyperbaric oxygen therapy
Hyperbaric therapy is a form of medical treatment that involves exposing the body to pure oxygen at a higher pressure than normal. There are about 45 diseases approved worldwide to be treated with hyperbaric oxygen.
READ MOREHyperbaric oxygen therapy in the management of patients with malignant otitis externa
Malignant otitis externa is a rapidly spreading bacterial infection that is aggressive and may be fatal if left untreated. Hyperbaric oxygen therapy (HBOT) is a medical treatment in which the entire body is placed in an airtight chamber at increased atmospheric pressure and has been proven to be effective for several different medical conditions.
READ MOREHyperbaric oxygen therapy in acute myocardial infarction
If left untreated, MI will lead to the progressive loss of viable cardiomyocytes, impaired heart function, and congestive heart failure. Oxygen cycling therapy serves as a very attractive option for the treatment of myocardial infarction, because it offers some of the greatest benefits while reducing treatment time and inconvenience to the subject.
READ MOREHyperbaric oxygen in ischemic ulcers
The present study has demonstrated that adjunct HBOT enhances the reduction of ulcer area and depth at 4 weeks in T2DM patients with ischaemic DFUs. HBOT is known to ensure hyperoxygenation of ischaemic tissue and restoration from hypoxia. Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest.
READ MOREHyperbaric therapy in femoral condylar osteonecrosis
Osteonecrosis of the knee (ONK) is a form of aseptic necrosis resulting from ischemia to subchondral bone tissue. Typically, treatment is invasive. Hyperbaric oxygen therapy (HBOT) may provide a noninvasive alternative by improving oxygenation and reperfusion of ischemic areas. This study evaluates the efficacy of HBOT in a series of ONK patients.
READ MOREHyperbaric therapy in femoral head necrosis
Femoral head necrosis (FHN), also called avascular necrosis, or femoral head osteonecrosis is a common multifactorial condition that affects patients of any age and can lead to substantial clinical morbidity. Hyperbaric oxygen therapy (HBO) is one of the proposed treatments. Indeed, tissue oxygen promotes angiogenesis that reduces edema. Read about the effectiveness of this treatment.
READ MOREHyperbaric oxygen therapy in central retinal artery occlusion
Central retinal artery occlusion (CRAO) is a devastating and common eye condition. It presents a sudden, unilateral, and painless loss of vision. Even when treated promptly, an acute obstruction of the central retinal artery usually leads to severe and permanent loss of vision.
READ MOREHyperbaric therapy in irradiated maxillofacial dental implant
There are numerous studies reported for the effectiveness of HBO in the treatment of osteoradionecrosis of various bone tissues. In addition to its usefulness in treating osteoradionecrosis, this therapy can prevent it. It also combats the negative effect of irradiation, stimulates osseointegration, and improves the survival rate of the implant.
READ MOREHyperbaric oxygen therapy in hear loss
The auditory function in the inner ear is maintained by the cochlea, which is known to have a high oxygen demand. Hyperbaric oxygen can increase the tension of oxygen in the perilymph and restore hearing in a significant number of patients with sudden hearing loss. Patients can be treated in a single-seater hyperbaric chamber or in a multiplace chamber.
READ MOREHyperbaric therapy in traumatic ischemia
Limb trauma, which leads to direct tissue damage, plus local hypoxic disorders caused by the resulting edema, causes acute peripheral ischemia. Surgical treatment and hyperbaric oxygen are not concurrent treatment modalities but are best used to complement each other in order to provide the best outcome for the patient.
READ MOREHyperbaric therapy in venous embolism
Small gas embolisms, as in this case, present serious risks, especially the complication of cerebral air embolism. To prevent neurological complications, it is necessary to urgently remove the air bubble. HBOT reduces the volume of the bubble, helps eliminate nitrogen, and improves the oxygenation of potentially hypoxic tissue. See the results of hyperbaric therapy in venous embolism.
READ MOREHyperbaric therapy in osteoradionecrosis
Osteoradionecrosis (ORN) is a common consequence of radiation provided to cancer patients. Currently, hyperbaric oxygen therapy (HBOT) has a major role in improving wound healing in patients with ORN.
READ MOREHyperbaric oxygen therapy in soft tissue radionecrosis
Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest, with multiple medical and anti-aging uses. The Baroks chamber has 5 seats, and operates at a constant pressure of 2.5 atmospheres, being fully automated and having protocols for each condition, and can be used individually for each patient.
READ MORESUCCESSFUL RECOVERY STORIES
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT