See details
READ MORE
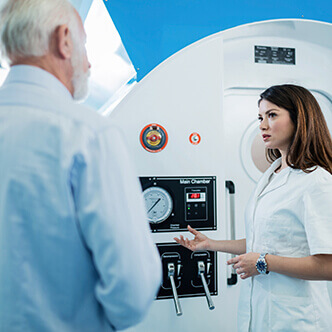
Hyperbaric oxygen therapy - benefits
Patients who use the clinic's hyperbaric therapy services benefit from:
- The only medically accredited hyperbaric therapy chamber in Bucharest, which operates at 2.5 atmospheres (those for aesthetic use go to 1 atmosphere and have no medical benefits).
- A safe medical procedure, without irradiation, without pain, without other side effects.
- The specialized medical team consists of recovery doctors, orthopedists, rheumatologists, neurologists, and neurosurgeons, meaning a multidisciplinary team specialized in all diseases that can be treated with hyperbaric therapy.
- Premium conditions at a fair price. Our clinic is recognized for the conditions offered and for the care of each patient. But we do not need to pay exorbitant prices to have access to quality medical services. At Centrokinetic you can find an affordable and fair price. But note that we do not have a contract with the National Health Insurance House (we do not offer state reimbursed services)
Centrokinetic is keeping contact with prestigious clinics and universities in Belgium, the Netherlands, France, and Greece to constantly update treatments to provide patients with the best medical solutions.
Causes of post-radiation central nervous system injuries
Increased use of radiation therapy and increased lifespan following radiation treatment has led to an increase in post-radiation central nervous system damage in patients who have previously undergone radiation treatment. At this time, treatment information for patients suffering from this very serious side effect is limited and not readily available. It is mandatory to respect the treatment options, to take into account the complications that may occur, and the success rate for these patients. The review and investigation of these conditions and the subjective results make the material of this study. It was determined that for patients who have post-radiation effects on the central nervous system it is important to designate a diagnosis first. For patients suffering from radionecrosis, the conclusion is that treatment with hyperbaric oxygen (HBO2) helps to improve the patient's condition and radiological results. However, the results were not similar in all patients. For patients with radiation-induced damage to the central nervous system, which occurs very late, HBO2 does not always provide a positive result, which means that classic treatment combined with HBO2 is needed to achieve the desired results.
Introduction
Hyperbaric oxygen therapy involves the use of so-called levels of oxygen under pressure to increase the level of oxygen in the blood. The use of hyperbaric oxygen therapy involves oxygen treatment for soft tissue radionecrosis. However, research is limited on the effects of HBO2 on post-radiation damage to the central nervous system in many patients. Because the central nervous system is another type of soft tissue, it is logical to consider from the beginning that HBO has a similar effect to that seen in other soft tissues. For example, brain tissue does not regenerate like skin. The brain may be deprived of blood flow after radiation damage, which means that the manifestation can be seen as a chronic ischemic condition, which can be resolved with HBO. There are several effects of HBO2 that doctors expect to lead to improved outcomes.
First, HBO2 provides a neuroprotective effect on cells by decreasing edema and ischemia. Second, HBO2 will decrease apoptosis at the site of ischemia by activating anti-apoptotic factors. Thirdly, it will help to form blood vessels for better irrigation of the ischemic area. HBO2 has also been shown to increase the stability of the brain barrier, which reduces the transfer of neurotoxic metabolites. Finally, HBO decreases inflammation at the site of necrosis, reducing myeloperoxidase activity, and ICAM-1 levels.
Previous reports of radiation therapy to the central nervous system show that there is an incidence of approximately 90% of neurotoxic lesions.
Kuffler and colleagues cite previous studies that show possible changes in MRI in the therapy of radiation-induced necrosis, as well as possible side effects. This cited study describes neurological deficits such as progressive dementia, memory loss, changes in vision or changes in hearing, and ataxia. However, due to limited information on the neurotoxicity of CNS radiation, more studies must be performed to determine more treatment methods.
Methods
The retrospective analysis of 10 patients with post-radiation central nervous system injury treated since 2000 and until 2011 at a hyperbaric unit is the object of the study. All patients were scheduled to receive 100% oxygen (O2) for 30 treatments, as most soft tissue radionecrosis conditions are treated in the range of 30-60 treatments - based on physician training and experience - at 2.4 absolute atmospheres for 90 minutes at each session. Deviations from this protocol are based on the individual situation of the patient. Patients who did not complete all 30 treatments, either refused additional treatment, could not complete treatment due to the disease or other factors, or it was decided that the treatments were not effective.
Patients who did not receive 2.4 atm abs received 2.0 atm abs. All these patients had contraindications using higher pressure in the hyperbaric chamber, such as a history of seizures or receiving concomitant chemotherapy. It is a well-known and common practice to reduce blood pressure while using chemotherapy due to the possibility of increased neurotoxicity. Chemotherapeutic agents that tend to generate increased toxicity include, but are not limited to, adriamycin, cisplatin, and bleomycin.
.jpg) | 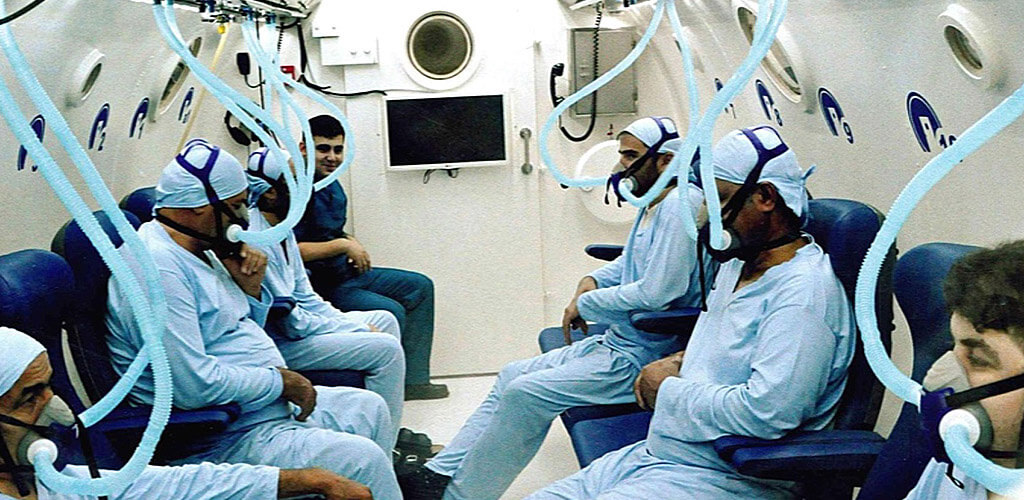 |
The study was approved by the Wisconsin Medical College Investigational Review Board (IRB). Patient information was kept secret and study sheets were not published. All published results involve a graphical review of the 10 patients qualified for the study, based on post-clinical evaluations and radiological images.
Descriptive statistics and a spreadsheet with relevant patient information and post-HBO2 therapy results were used.
A total of 10 patients (five men, five women) were treated between 2000 and 2011 for post-radiation damage to the central nervous system. The average age group was 58 years old. All patients were diagnosed with post-radiation lesions in the central nervous system.
The average dose of radiation received was 63 gray (Gy). The average duration before the presentation of encephalopathy was 39.8 months and the most common symptoms are headaches, loss of balance and coordination or vision changes, and neuropsychiatric changes.
HBO2 therapy was started after consent and all other standards of care treatments, such as steroids and chemotherapy, were continued.
The diagnoses were determined based on the analysis of images and radiological reports. Those patients who had an improvement in T1 on MRI were diagnosed with radiation-induced necrosis.
Patients without T1 improvement were diagnosed with radiation-induced encephalopathy. The result was determined by a careful review of the patient observation sheets.
Clinical results are shown by the patient's pre- and post-HBO clinical evaluation scores. These scores were reported by physicians throughout patient care and follow-up. The two clinical evaluations used by physicians were Karnofsky - Scale Performance Index Score and ECOG - Performance Score.
Subsequent comparative results before and after HBO were reported. For patients who had improvements, the results were noted separately.
These clinical evaluation tools are used to objectively monitor a patient's progress following the treatment regimen. Radiological outcomes were determined by a careful review of patient's radiology reports.
What are the effects of oxygen therapy on the body?
- Decreases inflammation
- Increases the body's oxygen saturation by 20-30%
- Increases the body's immunity
- Increases blood circulation and stimulates the formation of new capillaries
- Decreases toxins in the body
- Stimulates the production of new blood cells
- Increases healing rate
Results
The main purpose of this retrospective research study was to determine what are and whether there are significant improvements in the condition of patients with post-radiation lesions in the central nervous system through hyperbaric oxygen therapy. With this goal in mind, it has been established that the focus is on three categories of results. All these categories include subjective, clinical, and radiological results.
Previous case studies involving the treatment of radiation-induced necrosis or tumor resection, radiation-induced myelitis, or radiation following the treatment of arteriovenous malformation provided the baseline material to include these patients in the study.
Because these patients were observed in hyperbaric therapy by a certified neurologist, all data in the form of subjective and clinical outcomes come from the patient records that they completed before and after HBO2. Although not every patient submitted reports that included a clinical assessment tool, the primary assessment tools used are the Karnofsky or ECOG score.
The Karnofsky score classifies the patient's functional condition and the ability to take care of oneself. Scores range from 100% (no evidence of disease) to 0% (dead). The ECOG score also assesses the patient's functional status but focuses more on the impact of the disease on functionality. Scores range from 0 (fully active) to 5 (dead). Both clinical assessment tools can be used to track a patient's progress after treatment.
All radiological outcomes were determined by visualizing MRI imaging of the patient's central nervous system before and after treatment, and by reviewing relevant radiological reports.
Of these 10 patients, two had radiation-induced encephalopathy and one had radiation-induced myelopathy. While one patient with radiation-induced encephalopathy reported improvements in symptoms, three of the patients showed improvements including MRI.
Of the seven patients who were diagnosed with radiation-induced necrosis, three reported a subjective improvement in symptoms. For patient no. 1, the clinical evaluation remained stable after the HBO session. Patients no. 1 and no. 9 also showed an improvement in their radiological image, while patient 10 did not show imaging changes. Of the other four patients with radiation-induced necrosis, some indicated worsening of symptoms. Patient no. 4 had improved radiological images and patient no. 6 has not changed.
Notably, only two of these four patients underwent a full course of HBO2 therapy.
.jpg) | .jpg) |
Five of the ten patients had a history of seizure disorders. This could have affected the outcome of these patients due to the way the central nervous system was affected. With a history of seizure disorders, these patients received HBO2 at 2.0 atm because higher pressure could have affected the treatment outcomes.
Seven of the ten patients received concomitant steroid treatment when treated with HBO. Steroid treatment has been suggested as a treatment for radiation damage to the central nervous system. Therefore, these patients received treatment with steroids and HBO. This may have influenced the outcome for these patients and made it more difficult to determine the true effect of HBO treatments, although common practices indicate that steroid use is not known for how central nervous system pathologies are resolved but for relieving symptoms.
Five patients received concomitant chemotherapy during their HBO treatments. Patients 5 and 6 received chemotherapy which was a relative contraindication to HBO2 and therefore received HBO2 treatment at 2.0 atm which influenced their results because the standard procedure was changed.
These 10 patients represent 1.3% of all patients treated with HBO2 in the study period.
Below, their specific cases are described.
Case 1: A 71-year-old man with recurrent meningeal of the posterior fossa
He underwent resection and radiation therapy twice, in 1999 and 2004 (62 and 50 Gy). He later presented with progressive dysarthria, headache, and decreased coordination of his left arm. Karnofsky's score is 60% and the ECOG score 2 at the start. MRI of the brain shows "multifocal white and confluent in the frontoparietal and right side of the temporal region," a result described as leukoencephalopathy.
He was diagnosed with radiation necrosis of the brain. At approximately 24 to 36 months after receiving the radiation, he underwent three treatment sessions.
At the end of three rounds of treatment, the patient showed improved motor, oral, and gait function. HBO2 has improved his ability to move and use his arms. The new Karnofsky score was 50-60% and the ECOG score 2 to 3. MRI showed improvements. He died 25 months after completing treatment due to a progressive tumor.
Case 2: A 54-year-old man with an ACTH secretory pituitary adenoma
The tumor was resected and the patient received treatment with external radiation (50.4 Gy). He received 30 HBO2 treatments at 2.0 atm (due to a history of seizures) for vision loss in the left eye in 2006, with a reported improvement. As the tumor formed again, the resection was repeated twice. He suffered a repeated tumor after resection, continued to have low vision in his left eye. MRI showed the possibility of ischemia. Sixty-four months after radiation treatment, he underwent two HBO2 treatments for 90 minutes, each at 2.0 atm abs. After the two sessions, it was found that the vision did not change. MRI showed encephalomalacia in the left temporal pole. Because his condition did not improve, the patient gave up HBO and did not take a full course of treatment.
The patient underwent gamma radiation therapy for right cerebellar hemangioblastoma (70 Gy). He later reported ataxia and paresthesia of the left hand, paresthesia of the left leg, and ataxia of the right arm. He also accused instability and dizziness. The Karnofsky score was 70%, and the ECOG score 2 - 3. MRI showed lesions in the right pons and the right upper lobe of the cerebellum as well as another stable cerebellar lesion in the right lobe.
At 25 months after gamma radiation treatment, he received 28 HBO2 sessions at 2.4 atm for 90 minutes. After the therapy ended, worsening left-hand paresthesia and weakness, as well as worsening gait, were reported. The attending physician noted that “the patient is not sure if HBO helped. Karnofsky's score was 50 - 60%, and his ECOG score was 2 - 3.
MRI showed that in Varolio's bridge in the latero-posterior region the lesion was larger, with a cystic component, as well as a second lesion in the right lateral lobe which was larger. A new lesion was also present in the right lateral cerebellar hemisphere. He died 25 months after receiving HBO, the cause of death not being reported.
Case 4: A 68-year-old man with recurrence of atypical meningioma
The patient underwent resection of a meningioma on his left side, followed by a subsequent resection 15 years later. The surgery was complicated due to the infection and required a review. The patient had a recurrence and was treated with tomotherapy and radiation twice, once in 2005 and once in 2007 at 54 and 35 Gy.
At 32 months after completion of radiation treatments, the patient received 19 treatments with HBO2 at 2.0 atm (history of seizures) for 90 minutes each. After treatment, its functionality began to decline. The patient can no longer stand or feed on his own, and speech is also affected. At 52 months after HBO2 treatment, the patient survived. While the patient's condition and subjective evaluation could be done with a visit or a phone call, the stipulated IRB protocol is against this.
She also underwent chemotherapy for external radiation (50.4 Gy). He developed sensory changes in the lower extremities, weakness, difficulty walking, and urinary incontinence. MRI of the cervical and thoracic spine showed “replacement of the bone marrow with diffuse fat cells caused by radiation from T5 to T12.
At 12 months after radiation treatment, he underwent 30 treatments with HBO2 for 90 minutes at 2.0 atm (concomitantly with carboplatin and taxol chemotherapy).
After treatment, numbness was found to have improved, but the extreme weakness remained. He also continued to have incontinence.
The post-HBO Karnofsky score was 50%.
MRI showed the expansion of myelitis and diffuse bone marrow replacement in the vertebral bodies from T5 to L1. The patient died 4 months after the end of therapy.
Case 6: a 56-year-old woman with lung cancer metastases in the brain
The patient underwent gamma radiation twice (50.4 and 10.8 Gy, respectively). The patient's vision was reduced. The score of Karnofsky was 90-100%, and the ECOG score was 0-1. MRI showed focal improvement without appreciable inflammation or abnormality of the T2 signal inside a portion of the left optic nerve before the chiasm. Nine months after gamma treatment, she was sent for HBO2 therapy for optic nerve radionecrosis on both sides. She received two sets of 30 HBO treatment sessions at 2.0 atm (concomitant chemotherapy with carboplatin, pemetrexed, gemcitabine, and taxol) for 90 minutes, one set for each eye. After finishing therapy, he developed dysphagia and dyspnea. She was later hospitalized for pneumonia.
MRI showed stable changes in white periventricular matter and a decrease in the size of the right cerebellar lesion. After 54 months of treatment, it was concluded that the patient was alive.
Case 7: 43-year-old woman with lung cancer and brain metastases
The patient underwent complete radiotherapy and gamma treatment (40 and 21 Gy, respectively).
He had increasing headaches and gait imbalance, along with other neuropsychiatric changes that included depression, insomnia, and forgetfulness. Karnofsky score was 80-90%. MRI showed stable metastases in the right frontal and occipital lobes, as well as a vasogenic growth around both lesions. These findings were diagnosed as radiation-induced necrosis. At 24 months after receiving radiation, he received 30 HBO treatments at 2.0 atm abs (history of seizures) for 90 minutes. No data are available on the current clinical condition and there are no reported assessment scores. MRI revealed changes in the size of the lesion in the right anterior frontal lobe and a mass effect on the right side in the frontal horn with increased compression.
The patient received complete radiotherapy to the brain in 1999 and 2010 (30.6 and 38.5 Gy). He later developed seizures, dysautonomia, worsening dementia, changes in cognition and speech, and coordination difficulties. No ratings and scores were noted in her file. An MRI showed stable encephalomalacia in the right cerebellar hemisphere and multiple widespread lesions were observed in the brainstem. The patient was diagnosed with brain necrosis. At 24 months after receiving radiation therapy, he underwent 30 treatments with HBO2 for 90 minutes each at 2.0 atm (history of seizures). As a result of the treatment, she reported some improvements in gait and memory..
She continued to have thinking problems, seizures, and dysautonomia. Her neurologist did not report any clinical evaluation score, but in the evaluation sheet, she stated that she did not find any other positive effect of HBO2. MRI showed that the brain lesions did not increase in size. She died seven months after the end of HBO2 treatments, the cause of death being the massive effect of the tumor.
Case 9: A 38-year-old woman with an arteriovenous malformation of the left MCA
The patient underwent treatment with gamma radiation (21 Gy). He developed seizures, progressive headaches, gait imbalance, dysphagia, weakness on the right side, and reduced memory. Magnetic resonance spectroscopy showed necrosis at the site of radiation before therapy, and it was clinically diagnosed with radiation-induced necrosis. At 12 months after therapy, he received 30 HBO2 treatments at 2.0 atm abs (history of seizures). During treatment, he continued to have seizures, but no seizures were observed in the hyperbaric chamber. MRI shows the maturation and involvement of post-treatment effects in T1 decrease and post-contrast improvement in the left frontal lobe. While she reported some resolution of symptoms, she continued to have seizures, headaches, and gait imbalance. It has been established that these symptoms are not caused by the aggravation of radiation necrosis because it has provided improved imaging results. 65 months after the end of treatment, the patient was still alive.
Case 10: A 63-year-old man with meningioma of the right optic nerve sheath
The patient was treated with external beam radiation (40 Gy). He developed blurred vision, proptosis, and increased intracranial pressure. He was diagnosed with radiation-induced optic neuropathy. He received 30 HBO treatments at 2.4 atm for 90 minutes simultaneously, 19-31 months after the end of radiation treatment. Following therapy, he reported fewer symptoms. However, his ophthalmologist reported continuous ischemic disc swelling and secondary retinal edema. The ophthalmologist also noted that the patient continued to have high intracranial pressures as well as difficulty distinguishing colors. Repetition of the MRI did not report any change in meningioma. At 74 months after treatment, the patient was still alive.
Almost the entire sample of patients who have been diagnosed with radiation-induced central nervous system damage are those who have received head and neck radiotherapy treatments for CNS tumors.
As the field of oncology continues to evolve and the use of radiation is increasingly common, it is important to treat the patients who suffer from side effects of radiation therapy. Each of the new patients adds new data on necrosis or lesions that occur in the CNS.
Therefore, any information that doctors can extract about these patients is very useful and viable information for oncology and radiation therapy can help formulate a viable treatment.
Steroid treatments have a long history of serious side effects and disadvantages, including weight gain, soft tissue damage, and immunodeficiency. Because this option may not be available to patients with other co-morbidities, there is a definite need to find a new or adjuvant treatment option.
Radiation-induced encephalopathy in the CNS is a disease characterized by the appearance of a tumor, and edema of the brain. From an imaging point of view, this disease can be noticed by a lack of visibility of the white substance, although the changes are observed quite often.
Because encephalopathy is not due to tissue changes, it is considered that patients would have no major benefit from HBO therapy. Analyzing the patients in this study and their results, we see that this statement is correct.
Radiation necrosis of the central nervous system, on the other hand, has a completely different underlying pathology. Inflammatory reaction and subsequent necrosis of soft tissue is an ongoing problem. Once a single brain cell undergoes necrosis, the signals in that cell will cause other nearby cells to necrosis. Radiologically, necrosis of the nervous system is as visible as a tumor. Because this process is mediated by inflammation, it is thought that HBO2 therapy may be helpful for these patients. As the results of the study shows, patients with CNS radiation-induced necrosis show significant subjective improvements. It is believed that HBO2 therapy may be useful as a new treatment option for patients. An important benefit of HBO2 therapy is that treatment can be implemented on an outpatient basis. This makes the treatment easier, especially when given for long periods.
Oxygen is the element that codifies angiogenesis and fibroplasia in irradiated tissue and makes this dependent on the patient's condition. This has been determined by previous studies in which it has been shown that unirradiated but affected tissue is saved with the help of different doses of oxygen. Oxygen causes the irradiated tissue to be oxygenated spontaneously.
Following the information discovered in this study but also in other studies that preceded the conclusions on these 10 patients, it is important to take into account how to treat the lesions, with or without HBO. Radiation-induced damage to the central nervous system is in most cases labeled as the cause of brain radiation necrosis, which is the most feared complication associated with treatment for brain tumors. From a neurological point of view, the resulting signs and symptoms are often progressive and can be difficult to differentiate from a recurrent tumor.
Thus, if steroid treatment cannot remedy these complications, a therapeutic alternative such as hyperbaric oxygen should be considered. Given that endothelial cell damage and microvascular ischemia are among the manifestations of the radiation-induced disease, HBO2 is a valid therapy. This therapy does not reverse the manifestations, but the treatment can prolong the life of patients.
Not only the prolongation of life is important but also the improvement of its quality. Time is also a factor to consider when deciding on HBO2 treatment.

To date, it has not been justified that HBO immediately after radiation is not an effective treatment. If the patient has no lesions or signs and symptoms to show, there should be an indication for HBO. Radiation damage is progressively ameliorated and HBO treatment is a method that needs to be implemented.
Radiation injury therapy will be completed in the future, but HBO treatment is already proving to be viable as a standard plan due to the lack of side effects, unlike steroid and antithrombotic treatments.
Based on the results, it is concluded that HBO2 therapy can be used as a viable treatment option or as an adjunct treatment for patients with radiation-induced necrosis of the central nervous system. However, patient selection is important to find people who will respond positively to HBO2.
All patients who are evaluated for post-radiation should have an MRI to determine exactly what condition they have. Those patients who do not have imaging changes will be diagnosed with encephalopathy and are not recommended HBO2 therapy. Patients who have MRI changes should have additional tests because some changes may signal necrosis or tumor growth.
Because an MRI cannot distinguish between recurrent tumor and necrosis, these patients should ideally perform a biopsy of the lesion to determine its origin. If this option is not available, patients should have a PET scan. If the lesion is a tumor, then the PET scan will show hypermetabolic findings in the area. If the lesion is necrosis, hypometabolic results will occur.
Once the patient has been diagnosed with either a biopsy or a PET scan, he or she can be referred to HBO therapy.
Injury to the central nervous system should include HBO2 treatments and the use of these techniques which can be a completely effective tool but the patient should know that there is a possibility that positive results may not occur. All patients undergoing HBO2 treatment should be checked by their physician for any subjective, clinical, or radiological changes.
IN CASE YOU HAVEN'T ALREADY HEARD ABOUT US
Centrokinetic is the place where you will find clear answers and solutions for your motricity problems. The clinic is dedicated to osteoarticular diseases and is divided into the following specialized departments:
- Orthopedics , a department composed of an extremely experienced team of orthopedic doctors, led by Dr. Andrei Ioan Bogdan, primary care physician in orthopedics-traumatology, with surgical activity at Medlife Orthopedic Hospital, specialized in sports traumatology and ankle and foot surgery. .
- Pediatric orthopedics , where children's sports conditions are treated (ligament and meniscus injuries), spinal deformities (scoliosis, kyphosis, hyperlordosis) and those of the feet (hallux valgus, hallux rigidus, equine larynx, flat valgus, hollow foot).
- Neurology , which has an ultra-performing department, where consultations, electroencephalograms (EEG) and electromyography (EMG) are performed.
- Medical recovery for adults and children , department specialized in the recovery of performance athletes, in spinal disorders, in the recovery of children with neurological and traumatic diseases. Our experience is extremely rich, treating over 5000 performance athletes.
- Medical imaging , the clinic being equipped with ultrasound and MRI, high-performance devices dedicated to musculoskeletal disorders, and complemented by an experienced team of radiologists: Dr. Sorin Ghiea and Dr. Cosmin Pantu, specialized in musculoskeletal imaging.
Find the latest news by following the Facebook and YouTube accounts of the Centrokinetic clinic.
Oxygen therapy in diving accidents
Diving accidents are accidents that can occur during diving, being specific to this activity, and are always an emergency. Learn the benefits of hyperbaric therapy and why it is useful in diving accidents.
READ MOREContraindications Of Hyperbaric Oxygen Therapy
Hyperbaric oxygen therapy has multiple medical and anti-aging uses. Like any medical treatment, hyperbaric oxygen therapy has certain contraindications. Find out here what are the contraindications for hyperbaric oxygen therapy.
READ MOREThe Effectiveness of Hyperbaric Oxygen Therapy in Reversing the Aging Process in Humans
Scientists in Israel say they can reverse the aging process. The key to this success seems to be hyperbaric oxygen therapy – breathing pure oxygen while sitting in a pressurized chamber for a certain amount of time. In this case, it's 90 minutes/session, with a frequency of 5 sessions per week, for 3 months.
READ MOREHyperbaric oxygen therapy in intestinal pneumatosis
Cystoid or cystic intestinal pneumatosis (intestinal emphysema) is a symptom that can occur in many gastrointestinal diseases. Hyperbaric oxygen therapy can be a successful treatment of cystoid intestinal pneumatosis and granulomatosis with polyangiitis.
READ MOREHyperbaric oxygen therapy in cell damage caused by radiation in gynecological cancers
Gynecological cancers treated with a combination of external beam radiation and brachytherapy, especially cervical and vaginal cancers, can result in the apex of the vagina receiving a high dose of radiation. Hyperbaric oxygen therapy has positive effects on the radiated tissues, especially the head, neck, anus, and rectum.
READ MOREHyperbaric oxygen therapy in post-radiotherapy CNS injury
Hyperbaric oxygen therapy involves the use of so-called levels of oxygen under pressure to increase the level of oxygen in the blood. The use of hyperbaric oxygen therapy involves oxygen treatment for soft tissue radionecrosis. Read this article and find out more.
READ MOREHyperbaric oxygenation vs normobaric oxygenation in CO poisoning
Prolonged CO exposure is responsible for more than half of fatal poisonings and is also one of the leading causes of poisoning in Western countries. We aimed to compare the effectiveness of therapy with hyperbaric oxygen (HBO) versus normobaric oxygen (NBO) in the setting of carbon monoxide poisoning (COP).
READ MOREHyperbaric oxygen therapy in diabetic foot
Hyperbaric oxygen therapy may be effective for Wagner's grade 3 and 4 diabetic foot ulcers and need to study the real problems with patients seeking treatment and demonstrates the need to study the real problems with patients seeking treatment. The results show that it is important to follow the treatment in order for the HBOT to be efficient.
READ MOREThe role of hyperbaric oxygen therapy in sports medicine
Hyperbaric oxygen is used in sports medicine to reduce hypoxia and edema and is also effective in treating stroke injuries and acute traumatic peripheral ischemia. When used clinically, hyperbaric oxygen should be considered as an adjuvant therapy used as early as possible after the diagnosis of the lesions.
READ MOREHyperbaric oxygen therapy in muscle injuries
Muscle stretches are the most common muscle injuries suffered during performance sports. Rapid recovery from muscle injury is crucial for elite athletes who regularly are exposed to training and increased competition. Hyperbaric oxygen therapy is a safe and effective method, being a non-invasive treatment
READ MOREHyperbaric oxygen therapy in sports injuries
Hyperbaric therapies are methods used to treat disease or injury using pressures higher than the local atmospheric pressure inside a hyperbaric chamber. The long-term effects are neovascularization (angiogenesis in hypoxic soft tissues), osteoneogenesis, and stimulation of collagen production by fibroblasts. This is beneficial for wound healing and recovery after irradiation.
READ MOREHyperbaric oxygen therapy in proctitis generated by radiation
Proctitis is the inflammation of the rectal mucosa causing pain, discharge, and other unusual symptoms. Pain can occur during bowel movements, it can be acute or chronic. Symptoms may vary, but the most common is tenesmus (the feeling of needing to go to the toilet), a sensation that persists even after using the toilet. This treatment should be offered to patients who fail to recover with conventional treatments for radiation-induced proctitis.
READ MOREHyperbaric oxygen therapy in refractory osteomyelitis
Osteomyelitis is an infection of the bone or marrow caused by bacteria or mycobacteria. Hyperbaric oxygen treatments can be considered an American Heart Association (AHA) Class II recommendation for the treatment of chronic, refractory osteomyelitis
READ MOREHyperbaric oxygen therapy in tinnitus
Hyperbaric oxygenation allows a controlled increase in oxygen pressure in the blood. This technique can be used in cases of tinnitus and sudden deafness, when certain changes in the inner ear and brain generate a lack of oxygen and, therefore, a limited intake of energy.
READ MOREHyperbaric oxygen therapy of ischemia and reperfusion injury
Hyperbaric oxygen therapy has been found to ameliorate the damaging effects of reperfusion by early modulation of inflammation, maintenance of metabolic function in downstream tissues, and reintroduction of oxidation scavengers.
READ MOREHyperbaric therapy in the treatment of second degree burns
HBOT has a beneficial effect on burn wound healing by reducing edema and ensuring there is adequate oxygen in microcirculation. It may speed up epithelialization and suppress unnecessary inflammation that could negatively affect normal wound healing. With further research, HBOT may become an adjuvant therapy to surgery.
READ MOREHyperbaric oxygen therapy
Hyperbaric therapy is a form of medical treatment that involves exposing the body to pure oxygen at a higher pressure than normal. There are about 45 diseases approved worldwide to be treated with hyperbaric oxygen.
READ MOREHyperbaric oxygen therapy in the management of patients with malignant otitis externa
Malignant otitis externa is a rapidly spreading bacterial infection that is aggressive and may be fatal if left untreated. Hyperbaric oxygen therapy (HBOT) is a medical treatment in which the entire body is placed in an airtight chamber at increased atmospheric pressure and has been proven to be effective for several different medical conditions.
READ MOREHyperbaric oxygen therapy in acute myocardial infarction
If left untreated, MI will lead to the progressive loss of viable cardiomyocytes, impaired heart function, and congestive heart failure. Oxygen cycling therapy serves as a very attractive option for the treatment of myocardial infarction, because it offers some of the greatest benefits while reducing treatment time and inconvenience to the subject.
READ MOREHyperbaric oxygen in ischemic ulcers
The present study has demonstrated that adjunct HBOT enhances the reduction of ulcer area and depth at 4 weeks in T2DM patients with ischaemic DFUs. HBOT is known to ensure hyperoxygenation of ischaemic tissue and restoration from hypoxia. Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest.
READ MOREHyperbaric therapy in femoral condylar osteonecrosis
Osteonecrosis of the knee (ONK) is a form of aseptic necrosis resulting from ischemia to subchondral bone tissue. Typically, treatment is invasive. Hyperbaric oxygen therapy (HBOT) may provide a noninvasive alternative by improving oxygenation and reperfusion of ischemic areas. This study evaluates the efficacy of HBOT in a series of ONK patients.
READ MOREHyperbaric therapy in femoral head necrosis
Femoral head necrosis (FHN), also called avascular necrosis, or femoral head osteonecrosis is a common multifactorial condition that affects patients of any age and can lead to substantial clinical morbidity. Hyperbaric oxygen therapy (HBO) is one of the proposed treatments. Indeed, tissue oxygen promotes angiogenesis that reduces edema. Read about the effectiveness of this treatment.
READ MOREHyperbaric oxygen therapy in central retinal artery occlusion
Central retinal artery occlusion (CRAO) is a devastating and common eye condition. It presents a sudden, unilateral, and painless loss of vision. Even when treated promptly, an acute obstruction of the central retinal artery usually leads to severe and permanent loss of vision.
READ MOREHyperbaric therapy in irradiated maxillofacial dental implant
There are numerous studies reported for the effectiveness of HBO in the treatment of osteoradionecrosis of various bone tissues. In addition to its usefulness in treating osteoradionecrosis, this therapy can prevent it. It also combats the negative effect of irradiation, stimulates osseointegration, and improves the survival rate of the implant.
READ MOREHyperbaric oxygen therapy in hear loss
The auditory function in the inner ear is maintained by the cochlea, which is known to have a high oxygen demand. Hyperbaric oxygen can increase the tension of oxygen in the perilymph and restore hearing in a significant number of patients with sudden hearing loss. Patients can be treated in a single-seater hyperbaric chamber or in a multiplace chamber.
READ MOREHyperbaric therapy in traumatic ischemia
Limb trauma, which leads to direct tissue damage, plus local hypoxic disorders caused by the resulting edema, causes acute peripheral ischemia. Surgical treatment and hyperbaric oxygen are not concurrent treatment modalities but are best used to complement each other in order to provide the best outcome for the patient.
READ MOREHyperbaric therapy in venous embolism
Small gas embolisms, as in this case, present serious risks, especially the complication of cerebral air embolism. To prevent neurological complications, it is necessary to urgently remove the air bubble. HBOT reduces the volume of the bubble, helps eliminate nitrogen, and improves the oxygenation of potentially hypoxic tissue. See the results of hyperbaric therapy in venous embolism.
READ MOREHyperbaric therapy in osteoradionecrosis
Osteoradionecrosis (ORN) is a common consequence of radiation provided to cancer patients. Currently, hyperbaric oxygen therapy (HBOT) has a major role in improving wound healing in patients with ORN.
READ MOREHyperbaric oxygen therapy in soft tissue radionecrosis
Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest, with multiple medical and anti-aging uses. The Baroks chamber has 5 seats, and operates at a constant pressure of 2.5 atmospheres, being fully automated and having protocols for each condition, and can be used individually for each patient.
READ MORESUCCESSFUL RECOVERY STORIES
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT