See details
READ MORE
Recovery after reconstruction of the posterior cruciate ligament
Postoperative recovery usually lasts 6 to 9 months. The duration of each of the five phases of recovery and its total duration varies depending on the patient's age, the patient's physical condition, and the success of the operation. The first purpose of recovery is to protect the PCL graft by placing the knee in a movable orthosis fixed in full extension in the first weeks following surgery. The orthosis can be unblocked only during exercises to strengthen and recover the range of motion.In the first phase - passive flexion and active extension of the knee on a scale of 0-90 are encouraged. Also, isometric exercises of the quadriceps, lifting of the lower limb in extension, and stretching of the hamstring muscle are allowed.

These exercises are usually repeated 3 or 4 times a day, each series comprising from 10 to 25 repetitions. Knee edema should be closely monitored, as it contributes significantly to atrophy and muscle inhibition.
The main way to prevent knee edema is the RICE method: Rest, Ice, Compression, Elevation (Bed rest, local ice, compression, lifting the leg). Ice should be applied for 10-20 minutes every 2-4 hours, along with compression and lifting of the foot. To restore the extent of the movements and to prevent arthro-fibrosis, the patella must be mobilized in all directions immediately after the operation, in the early recovery phase.

In the next phase - the maximum protection phase - the range of motion should progress from 0 to 120 and the load should move from tolerable crutch loading to full loading without the aid of crutches. The following criteria should be met to stop using crutches:
- Good control of the quadriceps muscle
- No delays in stretching limb lifting exercises
- The full extension of the knee
- The ability to stand on one leg without pain
- No pain while walking.
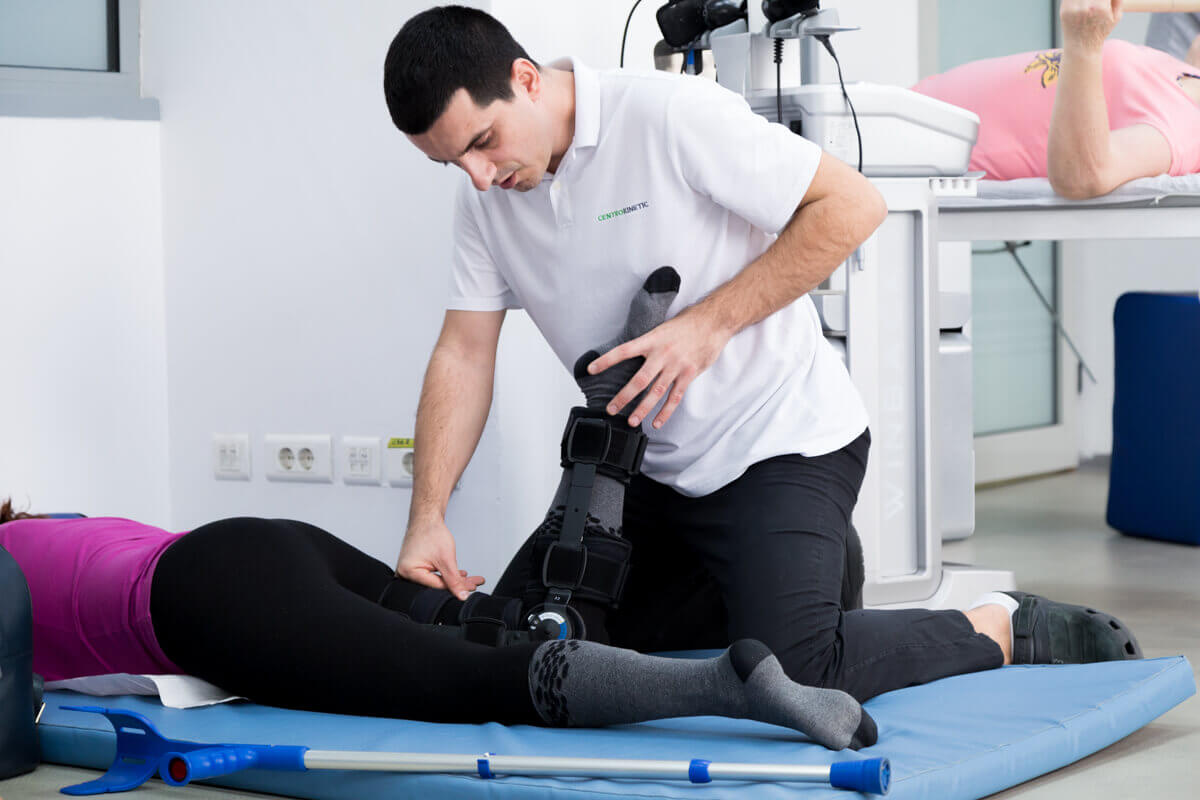
In this phase, it is also necessary to normalize gait, especially the loading and posture phases, by activating the quadriceps muscle. In this phase, the patient begins to perform open kinetic chain exercises to extend the knee joint (range from 0 to 70 degrees) and closed kinetic chain exercises (range from 0 to 45 degrees). Closed kinetic chain exercises include squatting exercises and uni- and bilateral press. Once the knee flexion is greater than 100, the patient can switch to stationary cycling. Hydrotherapy, limb lifting exercises with a maximum resistance of 10% of body weight, mini-squatting exercises (flexion of 0-45) can be incorporated as additional strengthening exercises. The RICE method should be continued in this phase as well.
In phase 3 - controlled walking phase - closed kinetic chain exercises progress from bilateral exercises to unilateral exercises with flexion of 45-60 degrees. Exercises such as wall squats, one-leg squats, or push-ups, which progress by adding resistance, improve the range of motion. In the first half of this phase, the patient should give up the knee orthosis. Balance and proprioceptive exercises, step-up exercises forward and sideways, band walking, and water jogging (pool hydrotherapy) are performed throughout this phase. The knee flexion exercises, with resistance, should be performed only at the end of this phase, due to the huge tearing force that PCL feels during this movement.

During phase 4 - light activity phase - progression is made from walking to easy running and light agility exercises are added to the program. These exercises include jumping and climbing trellis.
Progression from walking to jogging is possible if the patient meets the following criteria:
- Normal walk
- The range of motion of the knee is 0-120
- Lack of knee edema
- The ability to jump on one leg without pain
- Walking tolerance for at least 25 minutes
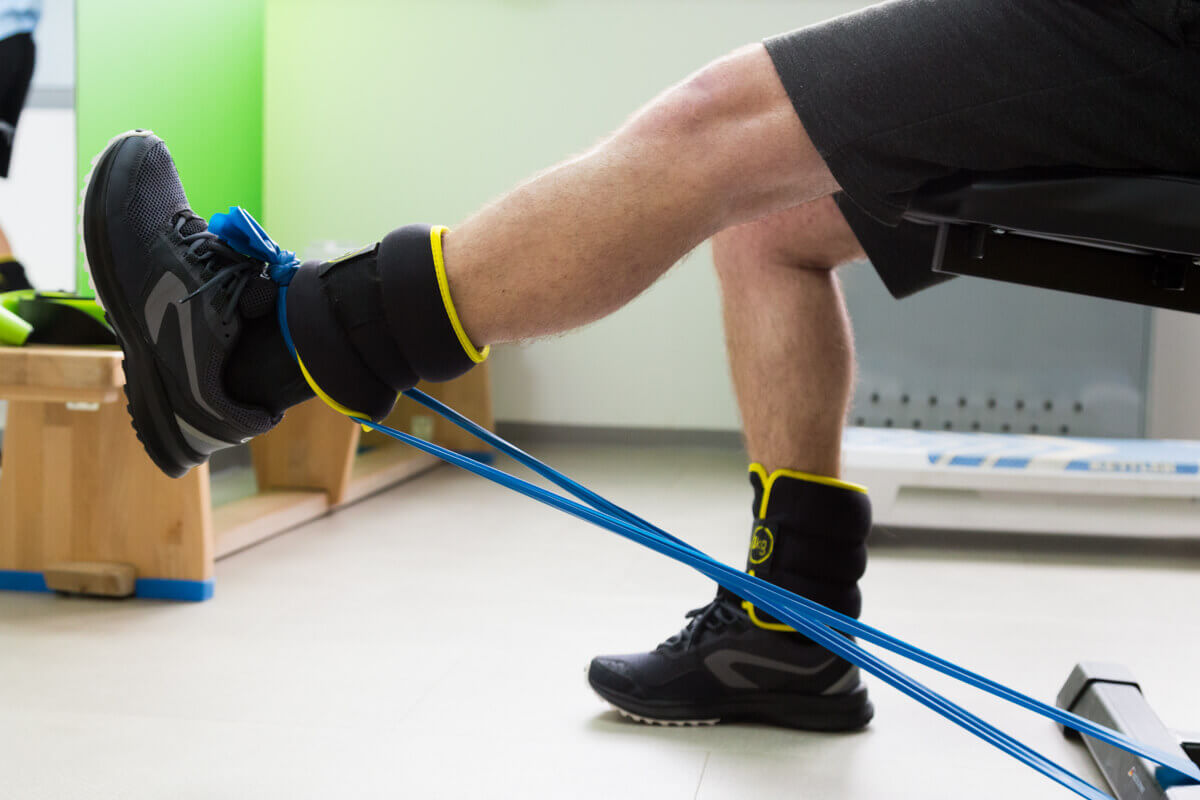
Knee and hip strengthening exercises should be continued and other exercises should be added to the program, such as open kinetic chain exercises of the quadriceps muscle (90-0 range), open kinetic chain exercises of the hamstring muscles (range 0 to 45 ), and closed kinetic chain exercises for marketing and casting (range 0-75). Swimming and agility exercises are initiated in the water, which will continue throughout this phase. Before returning to sports, the patient should be able to perform a jump test with a result of at least 80% of the ability to jump on the unaffected limb.

In the last phase of recovery - the return phase to sports activity- the intensity of strengthening exercises and the need for neuromuscular control increase. Examples of exercises in this phase include multi-directional squats, standing in a disturbed leg, running, change of direction exercises, and gymnastics. The activities specific to the sport practiced include movements in the sagittal, transverse and frontal planes. Closed kinetic chain exercises advance to a magnitude of 90, and open kinetic chain exercises of the hamstring muscle are now performed to a magnitude of 60. Strong impact exercises can also be performed two to four times a week. To determine whether or not the patient can return to sports, physiotherapists prefer the jump test. The result of the limb undergoing PCL reconstruction should be 90% of the result of the unaffected limb. During the test, jumping and landing should be monitored to avoid hyperextension or varus/valgus angulation.
At the end of the recovery period, the patient must be aware of the importance of the exercises he must perform at home. During sports activities, patients can use a functional orthosis to improve proprioception and to facilitate the correct mechanics of the knee during running and pivoting activities.

MAKE AN APPOINTMENT
CONTACT US
SUCCESSFUL RECOVERY STORIES
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT