See details
READ MORE
Recovery protocol in the operated frozen shoulder
A more precise way to define this is to refer to the true adhesive capsule (which affects the joint capsule) as a primary adhesive capsule. As the name suggests, the adhesive capsule affects the ligaments that surround the shoulder, but especially the joint capsule. In secondary adhesive capsule (or frozen shoulder) there may be some changes in the joint capsule, but the stiffness of the shoulders comes from something outside the joint. Some of the conditions associated with secondary adhesive capsulitis include rotator cuff rupture, biceps tendonitis, and arthritis. In any condition, the normally free parts of the joint capsule attach. This severely limits the shoulder's ability to move and causes the shoulder to freeze.
From my own experience, the frozen shoulder appears as an entity that generates major pain, exacerbated by tears at the slightest movement. It is a disabling condition for the patient.
Surgical treatment is not the first intention and is reserved for patients in whom conservative treatment has not brought any improvement in symptoms. It consists of procedures of joint distension under arthroscopic control or not, mobilization under anesthesia, or more elaborate arthroscopic interventions by synovectomy or even arthrolysis. A limited capsulotomy can also be performed, also by arthroscopic route, when the situation requires it. Manipulation under anesthesia can give very good results but should be avoided in patients with osteopenia or newly healed fractures.
Week 0 - 2
- Sling is allowed only for comfort, in the first 5-7 days, pulling the hand 5-7 times a day for elbow movement exercises (flexion/extension)
- Postural education and postural exercises
- Hand prehension exercises
- Apply ice every two hours for 15-20 minutes for the first 5-7 days, then 3 times a day.
- MPC (continuous passive movement) 4 - 6 hours a day for 1 - 4 weeks.
- Soft tissue mobilization focusing on the periscapular muscles, the cervical spine, and the rotator cuff.
- Scapular mobilization.
- Active and passive mobility movements to obtain a complete range of motion as fast as possible
- The cardio program may include a bicycle, treadmill, ergometer.

Week 2 - 4
- The full passive range of motion should be obtained in a maximum of 2-4 weeks
- Mobilization of the scapular and glenohumeral joint at the indication of the attending physician
- Start retraining and strengthening the rotator cuff, focusing on restoring proper biomechanics.
- Integration of the shoulder involves bilateral activities of the upper limbs and training to regain full range of motion (complete body movements that use both the upper and lower extremities).
- Continuation of the cardiovascular program and the basic one.
- Continuous application of ice 3 times a day.
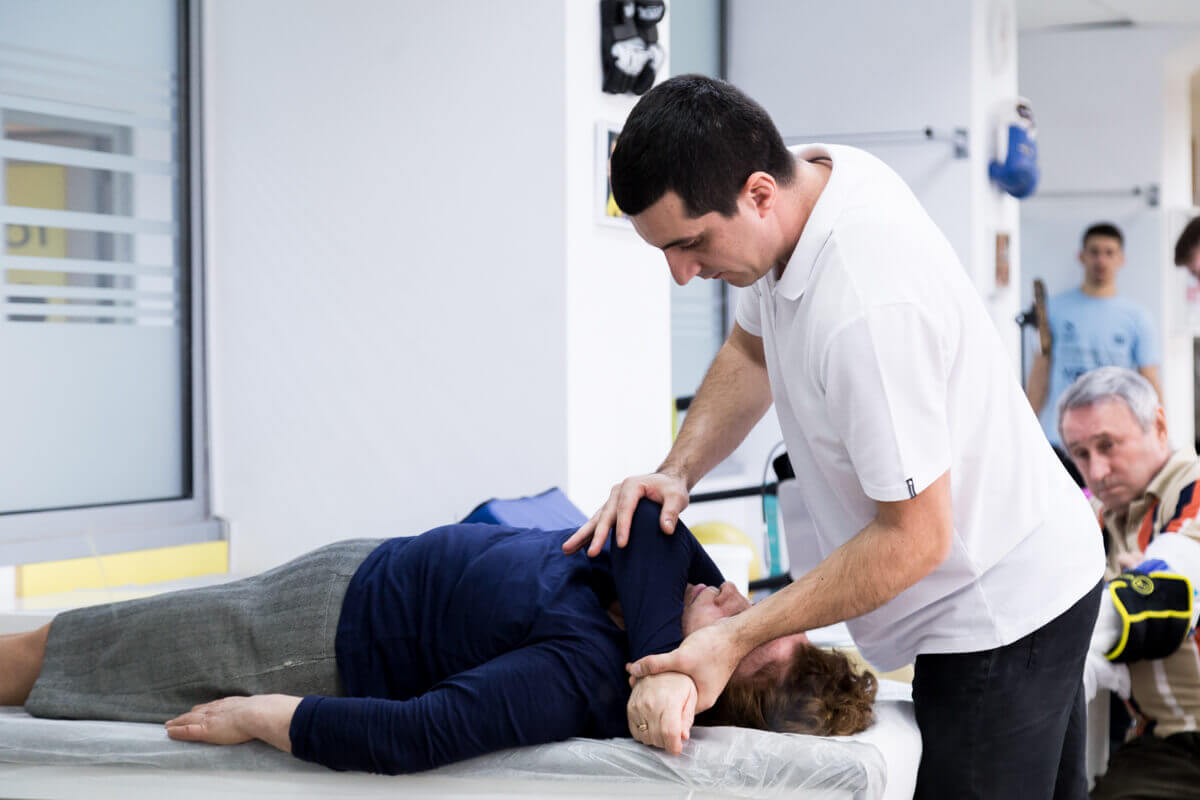
Week 4 - 8
- Progression of the strength program conditioned by a perfect biomechanics
- Development of an independent program for home and one for the gym.
- You can return to swimming after 6 weeks
Week 8 - 10
- Progression to normal activity in current activities and at work
- The patient is discharged with a lifelong maintenance program, including daily shoulder movement exercises, rotator cuff exercises, and cardio exercises.
SUCCESSFUL RECOVERY STORIES

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT





















































































































































