See details
READ MORE
Olecranon fracture recovery protocol
Olecranon fractures are among the most common pathologies of the elbow. Patients with olecranon fractures are unable to achieve elbow extension.These types of fractures are classified as some of the simplest intra-articular injuries. The surgical treatment and recovery process are relatively simple. Intra-articular fractures represent the majority of olecranon fractures and are generally associated with joint effusions and local hematomas. Extra-articular fractures include avulsion fractures and are most common in the elderly population.
Causes
The most common mechanism for producing these fractures is direct fall on the elbow or fall into the hands, with the elbow in hyperextension, the olecranon being thus pushed with force into the distal humerus.The second cause of olecranon fractures is triceps muscle contraction. The tendon of the triceps muscle is in intimate relationship with the periosteum that covers the olecranon, the contraction of this muscle causing an avulsion of the olecranon. This is the reason why some athletes, including gymnasts, who generate many isometric contractions of the arm have a high risk of developing these pathologies.
Treatment
The management of these fractures depends on the degree of displacement, comminution, and stability of the elbow. According to the Mayo classification, which incorporates these 3 variables, there are 3 types of fractures, each with 2 subtypes:- Fractures without displacement (type I) should be treated by simple immobilization and symptomatic treatment (analgesic/anti-inflammatory). Type I fractures are classified into non-comminuted and minimally comminuted. The patient is immobilized in an elbow splint for 2 weeks, after which active elbow movements begin, without resistance. Type II and III include displaced fractures, type II not presenting lesions at the level of the collateral ligaments, respectively type III which presents the interruption of the relationship between the forearm and the humerus.
- Type II and III are also subdivided into comminuted and non-comminuted fractures. The key difference between these fractures is represented by the fact that type III fractures are unstable, the instability of the elbow being given by the fact that in type III fractures there is a lesion of the medial collateral ligament. Thus, the most viable way to treat these fractures is the surgical one, by fixing them with plates and screws.
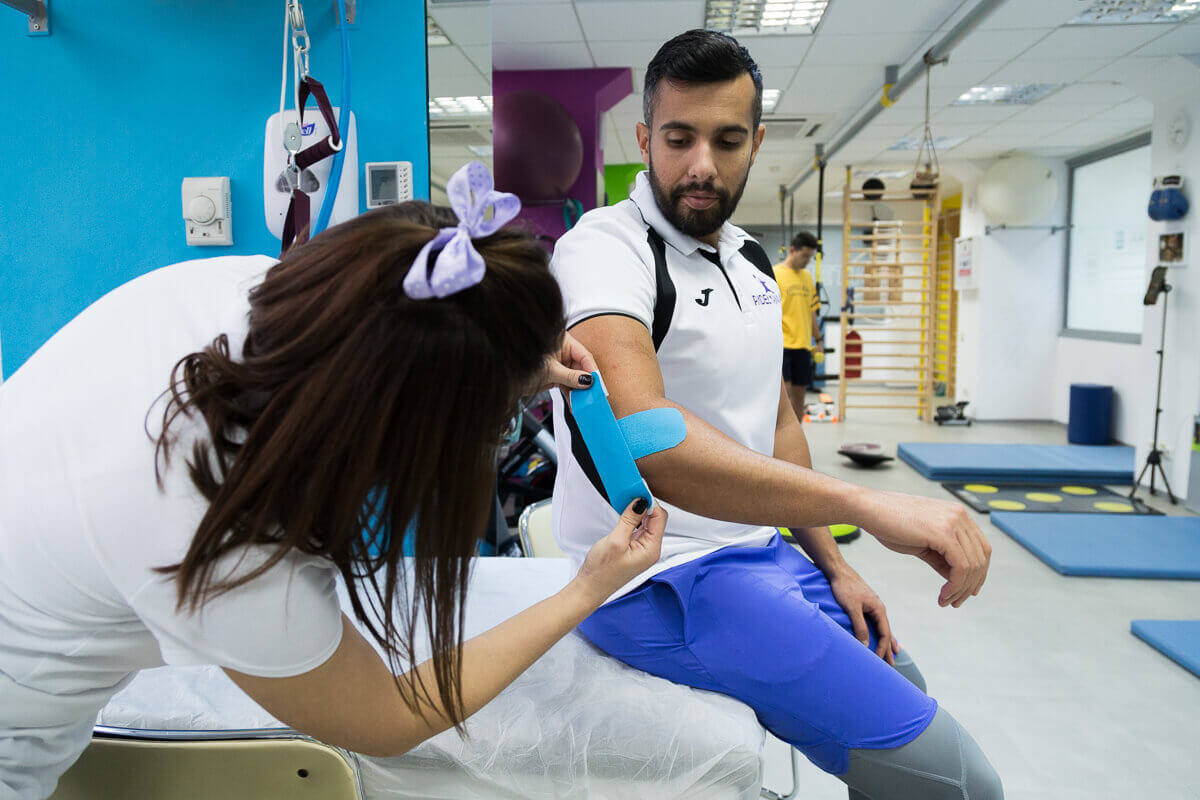
Post-surgery recovery protocol
Postoperative care is especially important for complete healing. The functional goal of the physiotherapist is to regain complete mobility of the elbow so that the patient can carry out his daily activities without problems, as before the trauma. However, there is a risk of a permanent loss of elbow extension. The recovery process and bone healing will take about 12 weeks.Week 1: Bone healing is in the inflammatory phase. The patient is immobilized in a plaster splint, bending 60 degrees, to minimize tension in the skin. The physiotherapist should check the capillary refill time, sensitivity, active and passive finger movements, and excessive swelling. Active movements of the elbow, hand, and finger mobilization can begin, with a splint. Fingers and hands may be swollen due to fracture. After 3-4 days, isometric hand exercises begin. Also now, slight elbow flexion movements and active fist mobilization movements begin, without splints.

Week 2: Bone healing is now in the repair phase. In most cases, the physical therapist begins isometric movements of the biceps and isotonic exercises of the fingers. At the end of the week, the cast is suppressed.
Weeks 4 - 6: The fracture is now partially stable. Active movements of mobilization of the shoulder, elbow, and fist are continued, under the careful supervision of the physical therapist. Isometric exercises of the elbow and hand, in flexion and extension, are now allowed. The patient can use the operated limb for his care.
Weeks 8 - 12: If the fracture is considered clinically and radiologically cured, the patient may begin to progressively use weights for elbow flexor and extensor exercises. The physical therapist continues the active mobilization of the elbow to the full extent of the movement, in all planes. There may be some restrictions on elbow extension, due to heterotopic ossification, in which case surgery is recommended for excision of excessive bone deposition.

SUCCESSFUL RECOVERY STORIES

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT





















































































































































