See details
READ MORE
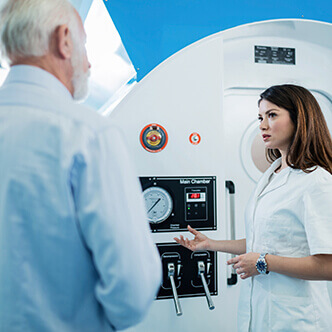
Discover the hyperbaric medicine center opened in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest, with multiple medical and anti-aging uses. The Baroks chamber has 5 seats, and operates at a constant pressure of 2.5 atmospheres, being fully automated and having protocols for each condition, and can be used individually for each patient.
Hyperbaric oxygen therapy - benefits
Patients who use the clinic's hyperbaric therapy services benefit from:
- The only medically accredited hyperbaric therapy chamber in Bucharest, which operates at 2.5 atmospheres (those for aesthetic use go to 1 atmosphere and have no medical benefits).
- A safe medical procedure, without irradiation, without pain, without other side effects.
- The specialized medical team consists of recovery doctors, orthopedists, rheumatologists, neurologists, and neurosurgeons, meaning a multidisciplinary team specialized in all diseases that can be treated with hyperbaric therapy.
- Premium conditions at a fair price. Our clinic is recognized for the conditions offered and for the care of each patient. But we do not need to pay exorbitant prices to have access to quality medical services. At Centrokinetic you can find an affordable and fair price. But note that we do not have a contract with the National Health Insurance House (we do not offer state reimbursed services)
Centrokinetic is keeping contact with prestigious clinics and universities in Belgium, the Netherlands, France, and Greece to constantly update treatments to provide patients with the best medical solutions.
What is carbon monoxide (CO)?
Carbon monoxide (CO) is a gas product of combustion, considered highly poisonous. Prolonged CO exposure is responsible for more than half of fatal poisonings and is also one of the leading causes of poisoning in Western countries.
Hyperbaric oxygenation vs normobaric therapy
We aimed to compare the effectiveness of therapy with hyperbaric oxygen (HBO) versus normobaric oxygen (NBO) in the setting of carbon monoxide poisoning (COP). We independently searched the National Library of Medicine’s Medline (PubMed™), ScienceDirect™, and Scielo™ for any relevant studies published from 1989 to 2017, using the following keywords: hyperbaric therapy, hyperbaric oxygenation, normobaric therapy, carbon monoxide poisoning, carboxyhemoglobin, Haldane effect. We analyzed the studies that suggested the effectiveness of HBO or NBO. Also, we searched for studies related to COP; including history, epidemiology (risk factors, incidence, demographics), pathophysiology, clinical manifestations, diagnosis, and treatment.
Sixty-eight articles were found, sixteen of which dealt with either HBO or NBO or both. Twelve suggested HBO as the treatment of choice in COP; four studies indicated that NBO was an adequate treatment due to its cost-effectiveness and availability in the emergency department (ED).
.jpg) | .jpg) |
HBO has been shown in several studies to be effective in moderate to high-risk COP situations, being the therapy of choice to avoid sequelae, especially neurologically. NBO can be considered as a reasonable alternative due to its cost-effectiveness. The availability and understanding of different therapeutic interventions are critical in the management of patients with COP in ED and the Critical Care unit.
Introduction
Carbon monoxide (CO) is a colorless gas, a product of combustion with no smell or taste. This gas is considered highly poisonous. Common sources for CO include malfunctioning heating systems, the exhaust of internal combustion engines, incomplete combustion of fuels, and inhaled smoke. High environmental concentrations of CO can be found in areas with poor ventilation and may cause signs and symptoms of intoxication.
Prolonged CO exposure is responsible for more than half of fatal poisonings, and is also one of the leading causes of poisoning in Western countries with several visits to the emergency department (ED) each year, just in the United States. Hyperbaric oxygen (HBO) and normobaric oxygen (NBO) have been suggested as the key therapeutic options with several controversies presented between different studies regarding methods, the number of patients, absolute atmospheres (ATA) given during HBO therapy, and overall clinical benefit.
One of the most widely quoted papers is the study by Raphael and colleagues who performed a randomized trial, assessing the controversial and debated topic regarding therapeutic advantages and indications in the treatment of CO poisoning with HBO, compared with the classical paramount management with NBO. Six hundred and twenty-nine adult patients were included in this study; inclusion criteria consisted of CO poisoning (COP) within 12 hours before admission. The studied population was divided into four groups based on the level of consciousness for which HBO and NBO were administered alone or in combination. The study concluded a reduction in neurological sequelae in those patients that sustained a loss of consciousness and attributed this effect to the wider use of HBO.
The clinical manifestations of CO poisoning are highly unspecific; these include headache, myalgia, dizziness (in severe exposures, confusion), loss of consciousness, and death. CO binds to hemoglobin 200-230 times more effectively than oxygen. This causes a leftward shift in the oxygen-hemoglobin dissociation curve, decreasing oxygen delivery to the tissues; the resulting tissue hypoxia has been proposed as the main mechanism of CO toxicity. CO additionally affects the cerebral perfusion through altered vasoactivity and neuronal responses independent of hypoxic stress. The resulting generation of carboxyhemoglobin produces a left shift dissociation on the oxygen-hemoglobin curve. This was, first described by Claude Bernard in 1865.
Prolonged CO exposure increases cytosolic heme levels, which leads to oxidative stress and binds to platelet heme protein and cytochrome c oxidase, which interrupts cellular respiration, causing increased reactive oxygen species generation leading to neural necrosis and apoptosis. Given its highly unspecific clinical presentation, CO poisoning remains one of the most challenging medical conditions to diagnose, the key element to this puzzle remains on the high level of suspicion that the physician must have based on a detailed history, including symptom duration and correlation with environmental CO exposure. Current methods to properly diagnose CO poisoning reside in the measurement of carboxyhemoglobin (COHb); it is a useful diagnostic method but is considered a weak indicator of the severity of poisoning, a consequence of the delay of the blood assay and timing of poisoning occurrence. The purpose of this article is to systematically review these two therapeutic interventions and compare their effectiveness.
History
The Greek and Roman empires made the first documented registry of CO application; both civilizations were familiar with this gas toxicity and found ways to apply its properties in the punishment of criminals. It was in 1880 when William Cruikshank described the main chemical properties of CO. In the middle of the 19th century, French physiologist Claude Bernard recognized that CO caused hypoxia by direct interaction with hemoglobin, and at the end of the century, Haldane studied the relationship between the high partial pressure of oxygen and its therapeutic effect on hemoglobin and CO.
Epidemiology
Prolonged CO exposure represents one of the most common causes of unintentional intoxication worldwide. It is mainly seen in a residential setting in the US and western countries. The high occurrence is confirmed by the Centers for Disease Control and Prevention (CDC) with an incidence of 23.2/million population per year and nearly 15,000 emergency department visits and 500 deaths each year in the United States alone. Most of the CO intoxications occur at home, and mostly involve females, children aged ≤17 years, and adults aged 18-44 years. On analysis of data regarding CO exposures, males represented an alarming 74% of unintentional non-fire related deaths and significant long-term morbidity, with an estimated 50% of neurologic sequelae in the non-fatal cases.
Pathophysiology
CO intoxication impairs oxygen delivery to tissues, resulting in cellular ischemia. It is explained by the tetrameric structure of the hemoglobin molecule and the affinity among the heme groups when the CO is bound at one of its four sites, which causes a left shift of the oxygen-hemoglobin dissociation curve and a hyperbola-like shape. The latter results in a hemoglobin molecule that has a decreased capacity to release oxygen to the tissues, including the respiratory center, leading to acidosis.
CO causes mitochondrial dysfunction due to binding to the cytochrome c oxidase, leading to worsening of hypoxia, and increasing the production of reactive oxygen species by alteration of the electron transport chain. In severe CO exposures (3000 ppm CO), the cAMP pathway has a deleterious role in ischemia-induced brain-damage.
What are the effects of oxygen therapy on the body?
- Decreases inflammation
- Increases the body's oxygen saturation by 20-30%
- Increases the body's immunity
- Increases blood circulation and stimulates the formation of new capillaries
- Decreases toxins in the body
- Stimulates the production of new blood cells
- Increases healing rate
.jpg) | 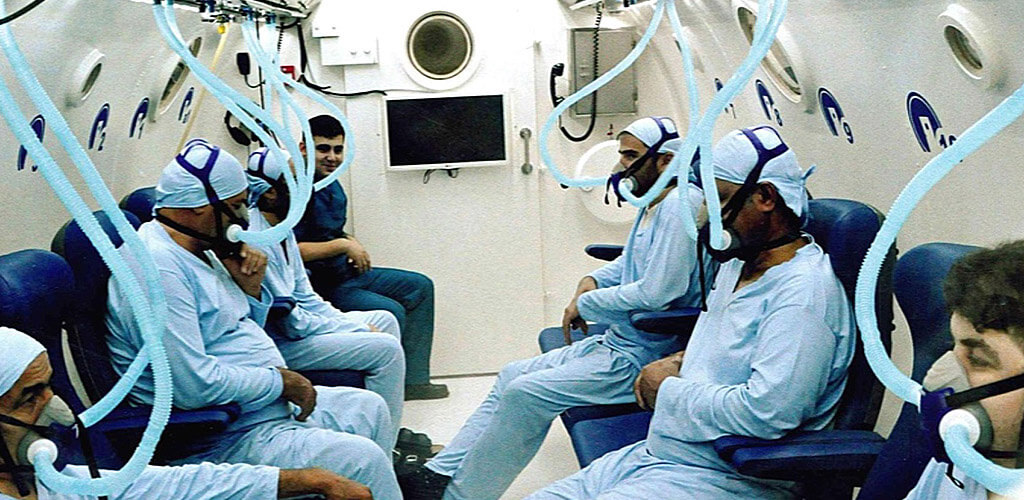 |
Clinical presentation
The symptoms of CO poisoning are usually nonspecific and can mimic a wide variety of disorders. Oxygen-dependent organs and those with low metabolic deposits show the initial signs of intoxication. The heart and brain are the first organs affected.
The severity of CO intoxication depends on several aspects: exposure to this gas, being the most important, the concentration of CO molecules in the air, and the level of COHb observed. In acute intoxications, a concentration below 1000 parts per million (ppm) and a COHb of 10% usually leads to headaches; concentrations above 1000 ppm and COHb of 20% cause dizziness, irritability, dyspnea, nausea, confusion, and syncope.
In patients with an exposure of 3000 ppm and more than 50% of COHb, convulsions, coma, and death occur after prolonged exposure. Myocardial lesions and fibrosis have been reported after chronic exposure to a moderate CO concentration; arrhythmias and sudden death (especially in patients with pre-existing heart disease) have been associated with acute CO exposure in the environment (up to 500 ppm).
Encephalopathy caused by exposure to carbon monoxide may cause cognitive impairment, memory loss, and neuropsychological symptoms for several days up to a few weeks after exposure.
Patients who die from carbon monoxide poisoning have a classic shade similar to the color of cherries, which is considered specific to patients intoxicated with carbon monoxide but can’t be assessed using this indicative level of intoxication.
Diagnosis
The diagnosis of COP rests in the high level of suspicion based on a detailed history of events, a key component of the initial assessment. Several diagnostic methods have been developed with the purpose of a rapid diagnosis, currently, the measurement of COHb by blood gas analysis represents the standard approach to a patient with a possible gas intoxication, several disadvantages of this method resulted from delayed blood assays and unavailability of first respondents in non-hospital scenarios have made clinicians look for other options for a timely diagnosis of the poisoning. In recent studies, the efficacy of CO oximeters and exhaled CO analyzers during the initial assessment have been remarkable in diagnosing the most severe poisoning cases in very short periods.
Data sources
This study protocol was prepared following the PRISMA guidelines. We sought to identify all relevant studies and documents that compared COP treatment by HBO and NBO methods. Our goal was to demonstrate the result with various therapeutic interventions. We searched electronic medical databases (PubMed, ScienceDirect, and Scielo) and excluded studies that did not provide outcome data.
The authors independently searched for relevant studies published from December 1989 to March 2017. All types of articles were consulted, including comprehensive reviews, potential observational studies, randomized controlled trials (RCTs), cross-group comparisons, editorials, retrospective studies. and case studies for relevant content analysis.
Data search
The following keywords were used: hyperbaric oxygenation therapy, normobaric oxygen therapy, carbon monoxide poisoning, carboxyhemoglobin, and Haldane effect. Articles were selected if they reported outcome data, as well as complications, sequelae, and/or mortality. The references cited in the selected articles were also independently reviewed and added for further analysis and comparison between HBO and NBO results.
Results
A total of 2124 articles were found from database searches and other sources and subsequently analyzed for any data on treatment for carbon monoxide poisoning with hyperbaric therapy and normobaric therapy. Only 16 clinical trials specifically addressed outcomes after HBO / NBO COP therapy. Twelve of them recommended HBO as the therapeutic intervention of choice in COP; four studies showed that NBO was a reasonable method due to its cost-effectiveness and availability in the emergency department.
Discussion
The non-specific clinical presentation of carbon monoxide poisoning involves a delayed diagnosis and treatment that represents a significant impact on the likelihood of short- and long-term neurological sequelae that are directly related to early cognitive decline.
In the last two decades, several studies have focused on accelerated diagnosis, which in turn leads to prompt treatments and possibly better results. The main controversy was whether to use HBO or NBO as a treatment.
Historically, Henshaw in 1662 first applied compressed air, trying to prove the HBO theory, but the experiment barely reached a pressure of 1.3 atm due to the inefficiency of his equipment. HBO therapy increases blood pressure and oxygen level and therefore improves the carbon monoxide detox, meanwhile, increasing the production of adenosine triphosphate (ATP), and reducing oxidative stress and inflammation.
The half-life of COHb is three to four hours for room air respiration, which is reduced to 30 to 90 minutes in the presence of a 100% oxygen concentration (normobaric oxygenation) and 15 to 23 minutes. with HBO at 2.5 atm.
HBO has been shown to significantly reduce the rate of complications, neurological sequelae, and mortality. In 1999, Camporesi demonstrated a decrease in mortality from 30% to 13.5% in a group of 213 patients; none of the patients treated with HBO suffered sequelae.
Garrabou and colleagues have shown that the effectiveness in recovering mitochondrial complex IV (mtCIV) function depends on the oxygen therapy administered. That being said, because HBO was more effective than normobaric oxygenation (NBO) in acute, moderate, and severe COP, an HBO session was effective enough to restore mitochondrial activity, reducing the rate of possible complications.
Research has concluded that the molecular effect of HBO results in the prevention of lipid peroxidation in the central nervous system and the preservation of ATP levels in tissues exposed to carbon monoxide, thus reducing damage. The results of the studies suggest that HBO may reduce the neurological/cognitive sequelae caused by carbon monoxide poisoning if given within 24 hours of an acute episode of CO poisoning.
Vomero and colleagues analyzed three clinical cases of CO intoxication in which the three patients were found unconscious; they mentioned that HBO must be applied under certain criteria, such as loss of consciousness, neurological disorders, or coma. If in this situation, the patient must be transferred safely and hemodynamically stable. A prospective study showed that the incidence of cognitive sequelae was lower in patients who underwent three HBO sessions within 24 hours after COP compared to patients treated with NBO.
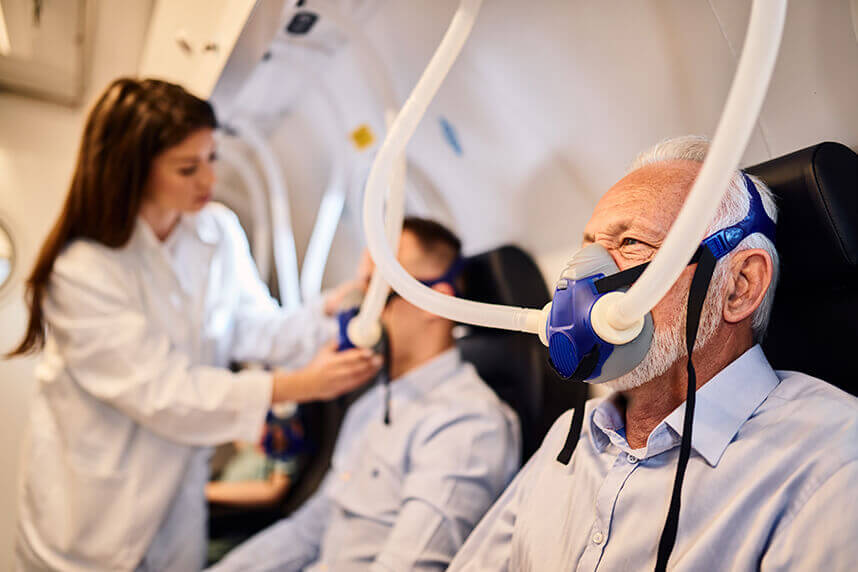
Undersea and Hyperbaric Medical Society recommends HBO therapy for patients with severe CO poisoning manifested by unconsciousness, abnormal neurological signs, cardiovascular dysfunction, such as myocardial infarction and acute coronary syndrome, severe acidosis, or patients older than 36 years. who have been exposed to carbon monoxide for more than 24 hours and who have a carboxyhemoglobin level of 25% or more.
Thom and colleagues conducted a randomized controlled study in 60 patients (divided into two groups) with mild-to-moderate COP in the first six hours after exposure. Neurological sequelae were observed in 23% of patients in the control group and none of the group receiving HBO treatment.
Ducasse and colleagues conducted a similar study in 26 non-comatous patients with acute COP divided into two groups. 12 hours after the treatment session none of the patients in the HBO group had abnormal clinical results, compared to the NBO group in which 5 of 13 patients had presented sequelae.
In 2017, Huang and colleagues showed that patients with CO intoxication who received HBO therapy had a lower mortality rate than those who received conventional treatment, especially patients under 20 years old and those with acute respiratory insufficiency. In this study, patients under the age of 20 with acute respiratory failure had a greatly reduced risk of death from HBO.
Also, a large-scale randomized controlled trial in Taiwan studied 25,000 patients with BPP over 13 years; 7,000 printed treatment using HBO-specific techniques and showed an improvement in mortality compared to patients who followed a standard therapy (NBO) protocol. Several studies involving patients with various clinical conditions indicated benefits and improvements in health in patients receiving HBO in 2 or 3 atmospheres, and one clinical study reported superior results in the administration of oxygen at a pressure of 3 atmospheres.
NBO speeds up the carbon monoxide detoxification and is a safe, readily available, and inexpensive method. If used as a single agent treatment, it must be provided until the carboxyhemoglobin level is less than 5%. Research results suggest that NBO may be less effective than HBO at preventing cognitive sequelae.
Sen and colleagues established that the treatment of CO intoxication first requires a high flux of 100% NBO until the normalization of COHb.
Another study by Scheinkestel sought to combat the use of HBO in CO poisoning. Patients received a 60-minute daily treatment at 2.8 atmospheres for three consecutive days for the HBO group in combination with prolonged high-flow oxygen therapy between treatments, while the NBO group received at least three consecutive days of continuous oxygen through the mask. facial. The authors attributed the unfavorable HBO result in higher doses of oxygen that could not add any additional benefit and could cause side effects. This study had a low follow-up rate (only 46% of patients participated in the entire study). We excluded this document from further analysis because no clinical assessment has been made of the sequelae of carbon monoxide poisoning.
Managing CO poisoning removes carbon monoxide from the body and increases the oxygen content of the blood by administering a high and concentrated flow of oxygen, while the patient is artificially ventilated and monitored.
Most studies analyzed in this research showed that HBO had higher therapeutic efficacy than NBO. HBO was suitable for life-threatening CO intoxications with COHb levels greater than 15% in patients with a history of loss of consciousness, neurological symptoms, pregnancy, or heart disease. Disadvantages of HBO therapy included barotrauma, hypoxic seizures due to a short supply of oxygen in a short period. It also includes the risks associated with transporting patients to treatment centers.
IN CASE YOU HAVEN'T ALREADY HEARD ABOUT US
Centrokinetic is the place where you will find clear answers and solutions for your motricity problems. The clinic is dedicated to osteoarticular diseases and is divided into the following specialized departments:
- Orthopedics , a department composed of an extremely experienced team of orthopedic doctors, led by Dr. Andrei Ioan Bogdan, primary care physician in orthopedics-traumatology, with surgical activity at Medlife Orthopedic Hospital, specialized in sports traumatology and ankle and foot surgery. .
- Pediatric orthopedics , where children's sports conditions are treated (ligament and meniscus injuries), spinal deformities (scoliosis, kyphosis, hyperlordosis) and those of the feet (hallux valgus, hallux rigidus, equine larynx, flat valgus, hollow foot).
- Neurology , which has an ultra-performing department, where consultations, electroencephalograms (EEG) and electromyography (EMG) are performed.
- Medical recovery for adults and children , department specialized in the recovery of performance athletes, in spinal disorders, in the recovery of children with neurological and traumatic diseases. Our experience is extremely rich, treating over 5000 performance athletes.
- Medical imaging , the clinic being equipped with ultrasound and MRI, high-performance devices dedicated to musculoskeletal disorders, and complemented by an experienced team of radiologists: Dr. Sorin Ghiea and Dr. Cosmin Pantu, specialized in musculoskeletal imaging.
Find the latest news by following the Facebook and YouTube accounts of the Centrokinetic clinic.
Oxygen therapy in diving accidents
Diving accidents are accidents that can occur during diving, being specific to this activity, and are always an emergency. Learn the benefits of hyperbaric therapy and why it is useful in diving accidents.
READ MOREContraindications Of Hyperbaric Oxygen Therapy
Hyperbaric oxygen therapy has multiple medical and anti-aging uses. Like any medical treatment, hyperbaric oxygen therapy has certain contraindications. Find out here what are the contraindications for hyperbaric oxygen therapy.
READ MOREThe Effectiveness of Hyperbaric Oxygen Therapy in Reversing the Aging Process in Humans
Scientists in Israel say they can reverse the aging process. The key to this success seems to be hyperbaric oxygen therapy – breathing pure oxygen while sitting in a pressurized chamber for a certain amount of time. In this case, it's 90 minutes/session, with a frequency of 5 sessions per week, for 3 months.
READ MOREHyperbaric oxygen therapy in intestinal pneumatosis
Cystoid or cystic intestinal pneumatosis (intestinal emphysema) is a symptom that can occur in many gastrointestinal diseases. Hyperbaric oxygen therapy can be a successful treatment of cystoid intestinal pneumatosis and granulomatosis with polyangiitis.
READ MOREHyperbaric oxygen therapy in cell damage caused by radiation in gynecological cancers
Gynecological cancers treated with a combination of external beam radiation and brachytherapy, especially cervical and vaginal cancers, can result in the apex of the vagina receiving a high dose of radiation. Hyperbaric oxygen therapy has positive effects on the radiated tissues, especially the head, neck, anus, and rectum.
READ MOREHyperbaric oxygen therapy in post-radiotherapy CNS injury
Hyperbaric oxygen therapy involves the use of so-called levels of oxygen under pressure to increase the level of oxygen in the blood. The use of hyperbaric oxygen therapy involves oxygen treatment for soft tissue radionecrosis. Read this article and find out more.
READ MOREHyperbaric oxygenation vs normobaric oxygenation in CO poisoning
Prolonged CO exposure is responsible for more than half of fatal poisonings and is also one of the leading causes of poisoning in Western countries. We aimed to compare the effectiveness of therapy with hyperbaric oxygen (HBO) versus normobaric oxygen (NBO) in the setting of carbon monoxide poisoning (COP).
READ MOREHyperbaric oxygen therapy in diabetic foot
Hyperbaric oxygen therapy may be effective for Wagner's grade 3 and 4 diabetic foot ulcers and need to study the real problems with patients seeking treatment and demonstrates the need to study the real problems with patients seeking treatment. The results show that it is important to follow the treatment in order for the HBOT to be efficient.
READ MOREThe role of hyperbaric oxygen therapy in sports medicine
Hyperbaric oxygen is used in sports medicine to reduce hypoxia and edema and is also effective in treating stroke injuries and acute traumatic peripheral ischemia. When used clinically, hyperbaric oxygen should be considered as an adjuvant therapy used as early as possible after the diagnosis of the lesions.
READ MOREHyperbaric oxygen therapy in muscle injuries
Muscle stretches are the most common muscle injuries suffered during performance sports. Rapid recovery from muscle injury is crucial for elite athletes who regularly are exposed to training and increased competition. Hyperbaric oxygen therapy is a safe and effective method, being a non-invasive treatment
READ MOREHyperbaric oxygen therapy in sports injuries
Hyperbaric therapies are methods used to treat disease or injury using pressures higher than the local atmospheric pressure inside a hyperbaric chamber. The long-term effects are neovascularization (angiogenesis in hypoxic soft tissues), osteoneogenesis, and stimulation of collagen production by fibroblasts. This is beneficial for wound healing and recovery after irradiation.
READ MOREHyperbaric oxygen therapy in proctitis generated by radiation
Proctitis is the inflammation of the rectal mucosa causing pain, discharge, and other unusual symptoms. Pain can occur during bowel movements, it can be acute or chronic. Symptoms may vary, but the most common is tenesmus (the feeling of needing to go to the toilet), a sensation that persists even after using the toilet. This treatment should be offered to patients who fail to recover with conventional treatments for radiation-induced proctitis.
READ MOREHyperbaric oxygen therapy in refractory osteomyelitis
Osteomyelitis is an infection of the bone or marrow caused by bacteria or mycobacteria. Hyperbaric oxygen treatments can be considered an American Heart Association (AHA) Class II recommendation for the treatment of chronic, refractory osteomyelitis
READ MOREHyperbaric oxygen therapy in tinnitus
Hyperbaric oxygenation allows a controlled increase in oxygen pressure in the blood. This technique can be used in cases of tinnitus and sudden deafness, when certain changes in the inner ear and brain generate a lack of oxygen and, therefore, a limited intake of energy.
READ MOREHyperbaric oxygen therapy of ischemia and reperfusion injury
Hyperbaric oxygen therapy has been found to ameliorate the damaging effects of reperfusion by early modulation of inflammation, maintenance of metabolic function in downstream tissues, and reintroduction of oxidation scavengers.
READ MOREHyperbaric therapy in the treatment of second degree burns
HBOT has a beneficial effect on burn wound healing by reducing edema and ensuring there is adequate oxygen in microcirculation. It may speed up epithelialization and suppress unnecessary inflammation that could negatively affect normal wound healing. With further research, HBOT may become an adjuvant therapy to surgery.
READ MOREHyperbaric oxygen therapy
Hyperbaric therapy is a form of medical treatment that involves exposing the body to pure oxygen at a higher pressure than normal. There are about 45 diseases approved worldwide to be treated with hyperbaric oxygen.
READ MOREHyperbaric oxygen therapy in the management of patients with malignant otitis externa
Malignant otitis externa is a rapidly spreading bacterial infection that is aggressive and may be fatal if left untreated. Hyperbaric oxygen therapy (HBOT) is a medical treatment in which the entire body is placed in an airtight chamber at increased atmospheric pressure and has been proven to be effective for several different medical conditions.
READ MOREHyperbaric oxygen therapy in acute myocardial infarction
If left untreated, MI will lead to the progressive loss of viable cardiomyocytes, impaired heart function, and congestive heart failure. Oxygen cycling therapy serves as a very attractive option for the treatment of myocardial infarction, because it offers some of the greatest benefits while reducing treatment time and inconvenience to the subject.
READ MOREHyperbaric oxygen in ischemic ulcers
The present study has demonstrated that adjunct HBOT enhances the reduction of ulcer area and depth at 4 weeks in T2DM patients with ischaemic DFUs. HBOT is known to ensure hyperoxygenation of ischaemic tissue and restoration from hypoxia. Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest.
READ MOREHyperbaric therapy in femoral condylar osteonecrosis
Osteonecrosis of the knee (ONK) is a form of aseptic necrosis resulting from ischemia to subchondral bone tissue. Typically, treatment is invasive. Hyperbaric oxygen therapy (HBOT) may provide a noninvasive alternative by improving oxygenation and reperfusion of ischemic areas. This study evaluates the efficacy of HBOT in a series of ONK patients.
READ MOREHyperbaric therapy in femoral head necrosis
Femoral head necrosis (FHN), also called avascular necrosis, or femoral head osteonecrosis is a common multifactorial condition that affects patients of any age and can lead to substantial clinical morbidity. Hyperbaric oxygen therapy (HBO) is one of the proposed treatments. Indeed, tissue oxygen promotes angiogenesis that reduces edema. Read about the effectiveness of this treatment.
READ MOREHyperbaric oxygen therapy in central retinal artery occlusion
Central retinal artery occlusion (CRAO) is a devastating and common eye condition. It presents a sudden, unilateral, and painless loss of vision. Even when treated promptly, an acute obstruction of the central retinal artery usually leads to severe and permanent loss of vision.
READ MOREHyperbaric therapy in irradiated maxillofacial dental implant
There are numerous studies reported for the effectiveness of HBO in the treatment of osteoradionecrosis of various bone tissues. In addition to its usefulness in treating osteoradionecrosis, this therapy can prevent it. It also combats the negative effect of irradiation, stimulates osseointegration, and improves the survival rate of the implant.
READ MOREHyperbaric oxygen therapy in hear loss
The auditory function in the inner ear is maintained by the cochlea, which is known to have a high oxygen demand. Hyperbaric oxygen can increase the tension of oxygen in the perilymph and restore hearing in a significant number of patients with sudden hearing loss. Patients can be treated in a single-seater hyperbaric chamber or in a multiplace chamber.
READ MOREHyperbaric therapy in traumatic ischemia
Limb trauma, which leads to direct tissue damage, plus local hypoxic disorders caused by the resulting edema, causes acute peripheral ischemia. Surgical treatment and hyperbaric oxygen are not concurrent treatment modalities but are best used to complement each other in order to provide the best outcome for the patient.
READ MOREHyperbaric therapy in venous embolism
Small gas embolisms, as in this case, present serious risks, especially the complication of cerebral air embolism. To prevent neurological complications, it is necessary to urgently remove the air bubble. HBOT reduces the volume of the bubble, helps eliminate nitrogen, and improves the oxygenation of potentially hypoxic tissue. See the results of hyperbaric therapy in venous embolism.
READ MOREHyperbaric therapy in osteoradionecrosis
Osteoradionecrosis (ORN) is a common consequence of radiation provided to cancer patients. Currently, hyperbaric oxygen therapy (HBOT) has a major role in improving wound healing in patients with ORN.
READ MOREHyperbaric oxygen therapy in soft tissue radionecrosis
Discover the hyperbaric medicine center open in our clinic. Centrokinetic has the top-performing hyperbaric chamber in Bucharest, with multiple medical and anti-aging uses. The Baroks chamber has 5 seats, and operates at a constant pressure of 2.5 atmospheres, being fully automated and having protocols for each condition, and can be used individually for each patient.
READ MORESUCCESSFUL RECOVERY STORIES
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT