.jpg)
Discover the open MRI imaging center in our clinic. Centrokinetic has a state-of-the-art MRI machine, dedicated to musculoskeletal conditions, in the upper and lower limbs. The MRI machine is open so that people suffering from claustrophobia can do this investigation. The examination duration is, on average, 20 minutes.
Centrokinetic attaches great importance to the entire medical act: investigations necessary for correct diagnosis (ultrasound, MRI), surgery, and postoperative recovery.
Hallux rigidus or osteoarthritis, a lesion of the cartilage of the phalangeal metatarsus of the big toe. The characteristic of this condition is the fact that the patient can not bend (lift from the ground) the thumb - toes.
Hallux rigidus is a tear (osteoarthritis) that occurs at the base of the thumb and is a chronic condition that affects the biomechanics of the joint at the base of the thumb. It appears as a pain and a limitation of the dorsiflexion of the toe.
.jpg)
The main symptoms are:
- stiffening of the movement in the main joint of the thumb
- thickening/prominence which is especially noticeable on the dorsal side of the forefoot
- joint pain
The patient must perform an X-ray to be able to quantify the degree of wear of the joint.
.jpg)
Most often, the cause is multifactorial. This means a combination of reasons, partly inherited, partly related to previous activities/events. It can also occur as an endpoint of inflammatory arthritis, such as rheumatoid arthritis or gout. However, in most people, it has nothing to do with these conditions. Occasionally, it occurs as a direct result of a joint injury. It is certainly possible to have hallux valgus and hallux rigidus at the same time.
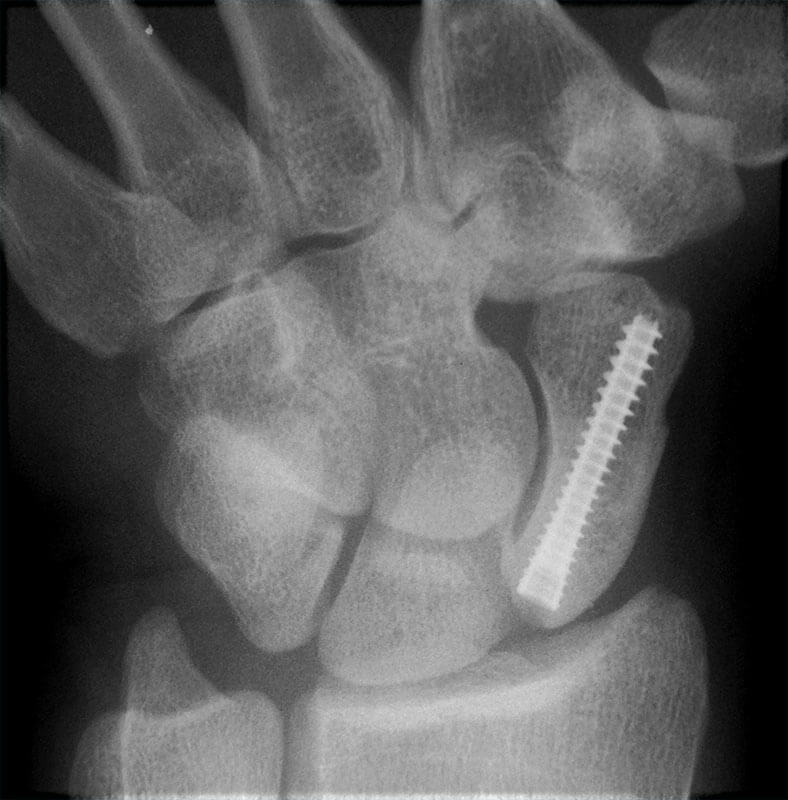
Surgical technique
There are several surgical approaches. The nature of the surgery is generally decided by the patient's age, the degree of physical activity, and the type of activity he practices, but also by the symptoms, their intensity, and their characteristics. For example, if they are easy, then we think of a simple, quick intervention, with the reintegration of the patient's family, social and professional, in a short time.
If arthritic symptoms are more problematic, the main intervention should be more complex, more invasive, to have the desired result.
There are 3 surgical techniques:
Joint debridement: there is no rapid assessment system or an objective assessment of symptoms, radiographs, and clinical signs to allow the unequivocal identification of patients who will benefit from the technique, which have an absolute indication. In general, however, the type of patient who can benefit from this intervention does not have advanced osteoarthritis, has good joint mobility, is young, active. An incision of about 2-3 cm is made in the superomedial area of the forefoot, centered on the affected joint. The joint is inspected, osteophytes are identified and the joint edges are regularized. The technique being minimally invasive, it is allowed to load the next day after the intervention, without crutches or metal frame.
.png) | .jpg) |
Arthroplasty: Replacing the joint at the base of the thumb has a long history, but the technique is still evolving. The purpose of the intervention is to maintain the mobile joint, maintaining a good mechanical function of the foot.
There are different surgical options and adapted prostheses: total arthroplasty in which both joint surfaces are replaced, replacement of a part of the joint (hemiarthroplasty), or silastic joints with hinges, where there is a flexible continuation of a spacer material in the joint space.
.jpg)
This procedure is used for advanced osteoarthritis in patients who do not want an arthrodesis. An arthroplasty has the advantage of maintaining minimal movement in the joint (although its practical effects are not so great, compared to a fusion of the thumb). The operation has a special advantage, that there is the possibility to wear heels postoperatively. The disadvantage of the procedure is that, as with all arthroplasties, the prosthesis eventually deteriorates and needs to be replaced, and the time varies depending on use, weight, and type of arthroplasty.
.png)
Postoperative
After the operation, the patient remains hospitalized for 1 day. He will receive pain medication and antibiotics during hospitalization. The operated limb is not immobilized, and the patient is advised to make ankle exercises, from the first postoperative day. Free walking is allowed immediately, without the need for crutches, given that the chosen intervention was joint debridement. In the case of arthrodesis, patients will wear a compressive bandage on the foot for 5 days and will use a special shoe when walking, which correctly distributes the body weight. Patients can return to daily activities quickly, up to 3-4 weeks.
At home
Although recovery after this operation is much faster than a classic intervention, it will still take a few weeks for you to fully recover the operated joint. You should expect pain and discomfort for at least a week postoperatively. You can use a special ice pack, which will reduce the pain and inflammation. You must be careful not to lean on the operated area in the first weeks because the pain and discomfort can worsen. You can take a bath, but without wetting the bandage and incisions. The threads are suppressed at 14 days postoperatively.
At 6 weeks postoperatively, an X-ray is necessary to see how the affected joint heals. Driving is allowed after 6 weeks, and hard physical work after 12 weeks.
Physical therapy plays a very important role in the rehabilitation program, and the exercises must be followed by a physical therapist until the end of the recovery period.
It is very important to follow the recovery program strictly and seriously for the surgery to be a success. Our medical team works on average with the patient after this intervention, 18-24 weeks until complete recovery of the operated area.
Following any surgery, medical recovery plays an essential role in the social, professional, and family reintegration of the patient. Because we pursue the optimal outcome for each patient entering the clinic, recovery medicine from Centrokinetic is based on a team of experienced physicians and physical therapists and standardized medical protocols.
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT




















































































































































