See details
READ MORE
- Basic information about gonarthrosis
- Causes and risk factors for gonarthrosis
- How gonarthrosis manifests itself
- How to diagnose gonarthrosis
- Treatment of gonarthrosis
- Drug treatment for gonarthrosis
- Surgical treatment for gonarthrosis
- Natural treatment for gonarthrosis
- Regenerative cell treatment for gonarthrosis
- Hyaluronic acid infiltrations for gonarthrosis
- Physical therapy in gonarthrosis
- Prevention of gonarthrosis
- Beneficial exercise in gonarthrosis
- Diet and nutritional supplements to prevent gonarthrosis
- Recommended spas for treating gonarthrosis
Article by dr. Georgiana Tache, primary care physician, with over 30 years of experience, vice president of the Romanian Society of Rehabilitation Medicine.
Basic information about gonarthrosis
Gonarthrosis or osteoarthritis of the knee joint is a degenerative disease of the joints, caused by the degeneration of the cartilage until its destruction, resulting in joint deformity; thus, less severe inflammatory reactions are secondary phenomena, arising from degenerative processes. In more than half of the cases where one knee is affected, both knees will have gonarthrosis.The onset of the pathology is usually associated with structural changes in cartilage tissue at the molecular level. Then, the process involves hyaline cartilage, which becomes cloudy, has a reduced thickness, and is covered with layered and mixed microscopic cracks. The pathological process results in the final destruction of the small and large cartilage and, at the same time, the exposure of the bone joint. The body reacts instinctively to the disappearance of cartilage through bone growth in peripheral areas, which leads to the growth of osteophytes.
Causes and risk factors for gonarthrosis
The major risk factor is being overweight. Being overweight or obese plays a major role because it is enough for the body mass index to be higher than 27 for the risk of developing osteoarthritis of the knee to be multiplied three times.Playing top sports is another known risk factor. Contact sports (especially football and rugby) expose the knees to serious injuries.
Meniscus removal (partial or total) and knee deformity are two other risk factors for the development of osteoarthritis.
Other causes that can lead to gonarthrosis:
- metabolic disorders
- especially hormonal imbalances
- knee injuries (fracture, cracked bones, torn ligaments, or meniscus)
- inflammatory diseases (rheumatism, arthritis)
- prolonged frequency and physical overload (especially in athletes - gymnasts, football players)
- endocrine disorders
- genetic abnormalities of tissue structure
- age factors
How gonarthrosis manifests itself
The pain that occurs during movement causes the patient suffering from gonarthrosis to save the affected limb by limiting physical and often professional activity, which leads to restricted mobility in the joint and even contracting in a bent position. In the later stage of the development of the disease, the pain takes place at rest, and the contour of the joint is permanently thickened and deformed.While walking, the patient rotates the lower limb outward, bends, and tilts the torso forward and sideways. The length of the step is then reduced, and the use of diseased lower limbs is limited. In the early stages of the development of degenerative changes, the patient does not feel symptoms and does not show any dysfunction. However, over time, mild and often unnoticed symptoms may occur, such as:
- difficulty performing knee flexion and extension in the full range
- slight swelling caused by effusion and thickening of the synovial
- redness and elevated temperature in the knee joint area, especially after exercise or other activities
- sensitive compression - characteristic cracking during movement, caused by the joint surfaces rubbing against each other
- quadriceps femoris muscle atrophy (especially the medial head)
- stiffness in the morning
When the degenerative process has already reached the advanced stage, the symptom of pain appears. In fact, the appearance of pain is the main reason why the patient goes to the doctor. The pain increases, especially when the affected person walks, stands for a long time, bends down, gets up from the chair, goes down the stairs, carries heavy objects.
The pain is located especially in the front or middle part of the knee joint. The pain that occurs during the movement makes the patient avoid the movement of the affected limb by limiting his physical and professional activity, which leads to restricted mobility.
![diagnosticare gonatroza]()
How to diagnose gonarthrosis
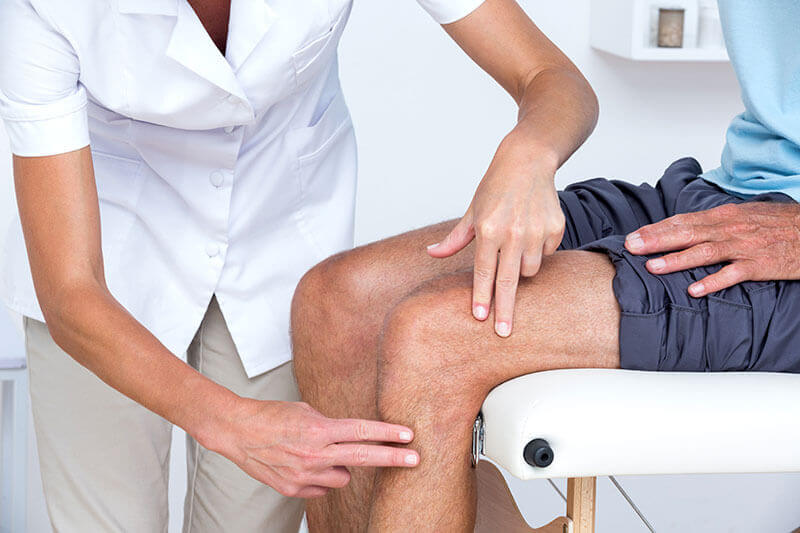
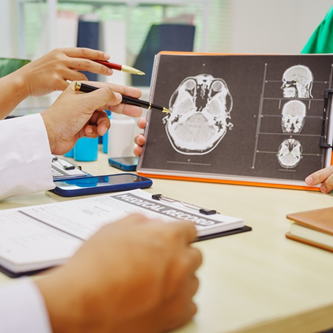
Degenerative changes in the knee joint are normally diagnosed based on imaging. The presence of osteophytes, ie the growth of bone on the joint bone of the femur and tibia, is the main diagnostic criterion for gonarthrosis. Osteophytes irritate adjacent tissues, causing inflammation. Through radiological images of the knee joint affected by the degenerative process, the stenosis of the articular surfaces can be observed, as well as the presence of free intra-articular bodies and the deformation of the articular axis. The primary diagnosis is made by inspection, palpation of the joint, change of direction of the bones, mobility of the plumb joints.
Laboratory research is performed on common blood and urine tests: determining the sedimentation rate of erythrocytes, fibrinogen, urea, and other biochemical parameters, and ultrasound scanning of the knee joint. The most informative are X-ray examinations and magnetic resonance imaging. Only then does the doctor treat the disease.
MRI or CT imaging to diagnose gonarthrosis
Magnetic resonance imaging (MRI) provides a sensitive tool for examining all structures involved in the gonarthrosis process. While much of the MRI literature has previously focused on cartilage, there is advanced research on whole organ evaluation and includes features such as synovitis, bone marrow edema, and meniscal and ligament pathology.
Ultrasound imaging for the diagnosis of gonarthrosis
Ultrasound is an effective technique that can be performed in the examination room minimizing patient discomfort. This method facilitates the repeated examination of all peripheral joints. The real-time imaging capability of ultrasound not only allows dynamic evaluation of joints but also provides a dimensional aspect that is not achieved by static radiology techniques.
Knee Arthroscopy
Knee arthroscopy is a surgical technique that can diagnose and treat problems in the knee joint. During the procedure, the surgeon makes a tiny incision and inserts a camera (called an arthroscope) into the knee. This allows you to view the inside of the joint on a screen. The surgeon will start by making a few small incisions or cuts in the knee. He will use saline to extend the knee. This will allow him to see more easily inside the joint.
Arthroscopy can repair many knee problems, including gonarthrosis. There are limited risks to the procedure, and the outlook is good for most patients. The timing and prognosis of recovery will depend on the severity of the knee problem, and the complexity of the procedure required.
![tratament gonatroza genunchi]()
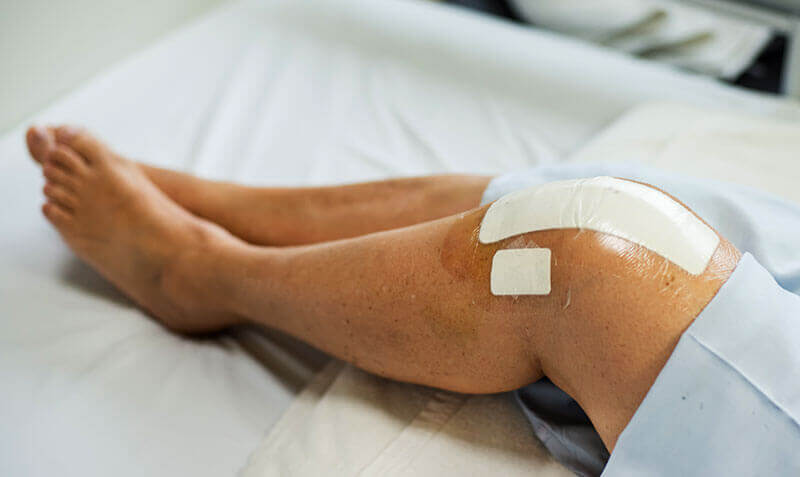
Treatment of gonarthrosis
The choice of the most effective treatment for gonarthrosis depends on the stage and factors that caused the disease. The goals of treatment include relieving pain and improving functioning. Drug treatment for gonarthrosis
Drug treatment should be followed for a long time to act on the disease, but watch out for side effects. Anti-inflammatory treatment will relieve joint pain and inflammation. The pills will not heal the diseased joint but will make life easier for the patient. To eliminate the pain, the patient must resort to massage and special gymnastics, thus activating the blood circulation process in the affected area. You can take food supplements such as chondroitin tablets and hyaluronic acid.Surgical treatment for gonarthrosis
If drug treatment does not bring impressive results, surgery is required. It is a radical method, but it restores the mobility of the joints. It is a safe and indicated method in advanced gonarthrosis, but it is recommended only for patients for whom other types of treatment have failed or are contraindicated. Damaged surfaces are removed, and the joint is replaced with titanium parts. This type of surgery helps eliminate pain, increases mobility, and improves the patient's life.The surgery is preceded by a complete examination of the patient, and by precise planning. The patient will perform medical tests, including EKG and blood tests. Depending on the individual arrangement, the surgery is performed under general anesthesia or by spinal anesthesia. Access to the affected joint is through an incision of about 15 cm in the front of the knee. After the surgery, it is necessary to perform an x-ray to check if everything is fine.
Natural treatment for gonarthrosis
To eliminate the pain caused by gonarthrosis, the patient must lose weight. A diet similar to the Mediterranean helps to restore cartilage. This diet contains foods rich in amino acids - fish, olive oil, fruits; vitamin C- oranges, tangerines, lemons, grapes, blueberries, salad, onions; Vitamin E - spinach, almonds, nuts, avocado, and natural oils; beta carotene - carrots and lysine, cheese, eggs, salt, beans, and dried fruits; Vitamin D - bread, milk, cereals, fatty fish, oysters; Vitamin A - liver, kidneys, dairy products, eggs, cod, sweet peppers, melons, tomatoes, broccoli, carrots, apricots, grapefruit and green vegetables. It is not advisable to consume too much coffee, meat, and alcohol, as they produce excess acid in the body. Creating acid in the body leads to inflammation of the joints.Gelatin is used as a supplement to desserts, as well as salty foods and salads. It is known as the best natural remedy for cartilage regeneration. Gelatin contains amino acids, proline and hydroxyproline, collagen, and does not contain fat and cholesterol, so there are no unwanted side effects when eating. You should include 10 g of gelatin daily if you want to use it to restore the cartilage of the knee. The gelatin treatment lasts 30 days, and then a 6-month break. You can buy gelatin from health food stores, but it is best to take beef gelatin.
The clay and lemon compress is very effective. Grind the seeds of two lemons, add 4 tablespoons of clay, and 1 egg white. Mix everything until you get a thick paste. Put the mixture on the gauze and put it on your knees. Tie tightly and let the compress act overnight.
Regenerative cell treatment for gonarthrosis
Cell treatment for regeneration is effective in treating gonarthrosis. They can be derived from a variety of tissues, but for therapeutic purposes they are collected from bone marrow or adipose tissue. They secrete bioactive molecules that stimulate angiogenesis and tissue repair and reduce T cell response and inflammation. This method of treatment was initiated in Romania by Dr. Andrei Ioan Bogdan in 2014 and remains a remarkable success in the field of orthopedics.Hyaluronic acid infiltrations for gonarthrosis
Intra-articular infiltrations with hyaluronic acid have received increasing attention in recent years, and have been shown to be particularly useful in the treatment of gonarthrosis, helping to improve joint function and reduce pain. The effectiveness of these infiltrations can be seen even after the first treatment, and their effects last over time. It is the treatment indicated for patients who reject the operation, and especially for those with 3 degree gonarthrosis, helping them to eliminate the pain. The frequency of this therapy is 1 vial every 6 months.![kinetoterapie gonartroza]()
Physical therapy in gonarthrosis
Physical therapy in gonarthrosis is an important component of treatment and should not be neglected. Physical therapy treatment comprises a set of exercises designed to strengthen the patient's health, customized to combat the disease. All therapeutic exercise schemes include the basic rules to avoid overloading, and to ensure maximum efficiency: - All movements are performed slowly and their amplitude gradually increases.
- The exercises take place daily. The total duration of physical exercises during the day should not exceed 35-45 minutes divided into 3-4 periods of 10-15 minutes each.
- Rest after each session should be at least 4 hours.
- Start the session by relaxing the leg muscles to improve blood flow.
Prevention of gonarthrosis
Disease prevention is very important. To prevent deformity of gonarthrosis, we must limit the weight placed on the knees and exercise. If you notice the first signs of illness, contact your doctor immediately. The sooner an examination of gonarthrosis is performed and treated, the better for the patient. You need to improve the condition of your knee ligaments, and to do this, you need to follow certain rules:- Wear comfortable shoes.
- Adequate nutrition.
- Regular exercises (especially cycling).
- Avoid putting heavy weights on the knee joint.
- Take vitamins.
Beneficial exercise in gonarthrosis
It is best to start physical therapy under the supervision of a therapist, but many patients with mild gonarthrosis do exercises that are explained in special textbooks or consult with gymnastics instructors. In any case, keep in mind the following recommendations:- Start slowly. It takes time to strengthen the muscles and make them more flexible, and a too fast increase in pregnancy almost always leads to injuries. Start with simple exercises and when the muscles become stronger, you will be able to gain weight.
- Don't ignore the pain. Gymnastics in gonarthrosis of the knee joint should not cause pain. You may feel discomfort when stretching your muscles, but if there is pain, you should stop exercising and let your muscles rest for a few days.
![prevenirea gonatrozei]()
Diet and nutritional supplements to prevent gonarthrosis
To prevent gonarthrosis, it is recommended to replace pork with chicken or turkey. This will allow the body to provide the necessary proteins. Don't forget the vegetable proteins, which are in large quantities in legumes. It is necessary to include in the diet the consumption of a small amount of nuts or almonds. 50% of all products consumed are raw vegetables and fruits. An extraordinary option is to make salads to which to add vegetable oil, yogurt, or kefir with low-fat content. i.Supplements containing glucosamine are among the most commonly used products for gonarthrosis. Although the evidence is not entirely consistent, most research suggests that glucosamine sulfate may improve gonarthrosis-related pain symptoms as well as slow disease progression.
Recommended spas for treating gonarthrosis
In order to prevent or treat gonarthrosis, treatment is recommended in balneoclimateric resorts with oligominerals, iodides, or sulfur. To benefit from these treatments and to partially or totally get rid of the pain, but also to correct the gait, patients can visit the following resorts in Romania:- Sulfurous waters: Herculane, Pucioasa
- Waters with oligominerals: Gioagiu, Felix
- Iodized waters: Govora, Bazna
- Chlorinated salt waters: Ocna Sibiului, Amara, Salt Lake
IN CASE YOU HAVEN'T ALREADY HEARD ABOUT US
Centrokinetic is the place where you will find clear answers and solutions for your motricity problems. The clinic is dedicated to osteoarticular diseases and is divided into the following specialized departments:
- Orthopedics , a department composed of an extremely experienced team of orthopedic doctors, led by Dr. Andrei Ioan Bogdan, primary care physician in orthopedics-traumatology, with surgical activity at Medlife Orthopedic Hospital, specialized in sports traumatology and ankle and foot surgery.
- Pediatric orthopedics , where children's sports conditions are treated (ligament and meniscus injuries), spinal deformities (scoliosis, kyphosis, hyperlordosis) and those of the feet (hallux valgus, hallux rigidus, equine larynx, flat valgus, hollow foot).
- Neurology , which has an ultra-performing department, where consultations, electroencephalograms (EEG) and electromyography (EMG) are performed.
- Medical recovery for adults and children , department specialized in the recovery of performance athletes, in spinal disorders, in the recovery of children with neurological and traumatic diseases. Our experience is extremely rich, treating over 5000 performance athletes.
- Medical imaging , the clinic being equipped with ultrasound and MRI, high-performance devices dedicated to musculoskeletal disorders, and complemented by an experienced team of radiologists: Dr. Sorin Ghiea and Dr. Cosmin Pantu, specialized in musculoskeletal imaging.
Find the latest news by following the Facebook and YouTube accounts of the Centrokinetic clinic.
SUCCESSFUL RECOVERY STORIES

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT