.jpg)
For all traumatic or chronic diseases of the musculoskeletal system, the Centrokinetic private clinic in Bucharest is prepared with an integrated Orthopedic Department, which offers all the necessary services to the patient, from diagnosis to complete recovery.
The Department of Orthopedic Surgery of Centrokinetic is dedicated to providing excellent patient care and exceptional education for young physicians in the fields of orthopedic surgery and musculoskeletal medicine.
Centrokinetic attaches great importance to the entire medical act: investigations necessary for correct diagnosis (ultrasound, MRI), surgery, and postoperative recovery.
Discover the open MRI imaging center in our clinic. Centrokinetic has a state-of-the-art MRI machine, dedicated to musculoskeletal conditions, in the upper and lower limbs. The MRI machine is open so that people suffering from claustrophobia can do this investigation. The examination duration is, on average, 20 minutes.
The patellofemoral complex, which consists of the medial and lateral femur-patellar ligaments, is the main passive stabilizer of the patellofemoral joint. Since rupture of the medial patellofemoral ligament (MPFL) is the main consequence of patellar dislocation and biomechanical studies have shown that MPFL is the major ligament that passively opposes patellofemoral instability and lateral patellar dislocation, MPFL reconstruction has become the main technique. to restore patellofemoral stability.
.jpg)
However, a recurrent patella dislocation must be investigated much more deeply to discover the causes of the recurrences. Most of the time, the recurrent dislocation of the patella is the consequence of some deviations of the biomechanical axis, of some patellofemoral dysplasias, or the high position of the patella (Patella Alta). Therefore, in these situations, MPFL reconstruction is not sufficient and other surgical techniques must be associated within the same surgery.
Returning to MPFL reconstruction, numerous surgical techniques for the reconstruction of the medial patellofemoral complex have been described, each with promising clinical results. However, since it is known that a non-anatomical reconstruction of MPFL can lead to non-physiological patellofemoral loads, the purpose of surgery must be anatomical reconstruction. Many studies have been performed to evaluate the femoral insertion of MPFL. Based on these anatomical, biomechanical, and radiological results, today there is the possibility of avoiding the complications of high patellofemoral pressure, which is associated with non-anatomical fixation of the graft (too anterior/proximal).
Our medical team uses three surgical techniques:
- From the gracilis tendon, fixed with two anchors on the patella and 1 screw on the femur
- From the quadriceps tendon, fixed with one screw on the femur
- From the large adductor tendon fixed with three stitches on the patella.
The gracilis muscle reconstruction technique through a double anatomical beam of the MPFL, provides good stability, both in flexion and extension. Also, the double anatomical beam technique successfully limits the excessive rotational movements generated by the instability of the joint. At the same time, executed correctly, the surgical technique has the benefit of a more aggressive recovery protocol, with the rapid professional and social integration of the patient.
An autograft (from the patient) of gracilis muscles can be used, its size and strength being sufficient for MPFL reconstruction (the approximate diameter is 4 mm). The minimum length of the graft must be 18 cm, with both ends sutured in tension (whipstitched 10 mm). The graft should also be narrowed at both chapels to facilitate easier insertion of the graft into the patella.
Surgical technique
The medial edge of the patella is palpated and an incision of 2 cm is made from the superomedial corner, which extends towards the center of the medial edge of the patella. Dissect to expose the medial edge of the patella. Using the fluoroscopic guide, at a point 3 mm distal to the proximal-medial corner of the patella, a channel with a minimum depth is drilled with a 2.4 mm guide brooch transversely along the bed. 25 mm. A second brooch, also of 2.4 mm, is positioned parallel to the first channel, at a distance of 15-20 mm. It is reamed with a cannulated drill of 4.5 mm, at a depth of 25 mm. Place one end of the graft through the hole/staple of the SwiveLock anchor and push the graft/anchor into the proximal canal until the staple is in the proper position. Maintain tension on the sutures and screw the SwiveLock anchor into the patella.
A determining factor in the success of MPFL reconstruction is the proper fixation of the femoral graft, our technique incorporating the use of a femoral template to ensure proper placement of the graft in the femur. This position ensures a static fixation point that equalizes the tension along with the graft, both in flexion and extension, thus minimizing the stress on the patellofemoral joint. With the help of an MPFL template, the appropriate position of the brooch is established. The entry point is approximately 1 mm anterior to the posterior cortex extension line, 2.5 mm distal to the posterior articular margin of the medial femoral condyle, and proximal to the posterior point of the Blumensaat line. The template was positioned on the area of the medial epicondyle of the femur, wherewith the help of the guide pin a 2.4 mm channel is made, along the femur and through the lateral epicondyle. Since the diameter of the gracillis muscle graft is about 4-5 mm in diameter, it is reamed with a 6 mm reamer.
The brooch is kept in the femur since it is used to pass the graft through the femur. The space between the medial vastus and the capsule is identified and dissected towards the femoral insertion area with the help of scissors, taking care not to perforate the capsule. A curved forceps is inserted towards the edge of the medial epicondyle and with the help of the tip of the forceps, a longitudinal incision of 1 cm is made. Using tweezers, pass a FiberWire wire with the loop to the patellar insertion area.
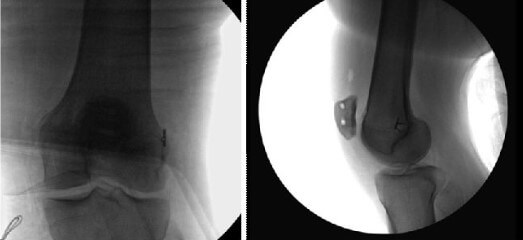
Pass the graft through the suture loop and pull from the patellar origin to the entry point of the medial epicondyle. It is imperative to maintain an equal tension in both chapels of the graft to ensure proper biomechanics of the patellofemoral joint. Remove the sutures through the medial incision and with equal tension on both ends of the graft, pull the graft towards the medial epicondyle.
A 1.1 mm Nitinol guidewire is placed next to the femoral guide to facilitate the insertion of the 6 mm x 23 mm bio-interference screw. Insert the sutures of the graft into the staple of a Kirschner brooch and run through the lateral femur, before inserting the graft into the femoral socket. Using clamp-like forceps, pre-tension the graft and insert it into the canal with equal tension on both ends of the graft. Manually fix the lateral patellar facet at the same level with the lateral femoral condyle, with the knee in flexion of 30 degrees. At this point in the operating time, it is possible to temporarily assess the graft isometry by maintaining adequate graft tension and by performing complete knee movements. Once the proper isometry of the graft has been established, complete fixation can be performed.
The operation lasts about 20-40 minutes, under spinal or general anesthesia. The anesthetist discusses with the patient, during the pre-anesthesia consultation, to evaluate the general state of health. Usually, the pre-anesthetic consultation is performed in the week before the surgery, when the patient's blood tests are also collected.
After the intervention, the patient is brought to the salon, and within 12 hours he can mobilize. In the next period, the foot should be kept up on a pillow, and an ice pack should be applied for 3-4 days. Postoperative treatment consists of antibiotic therapy, analgesics as needed, anti-inflammatory. The dressing is changed every 48 hours, and the threads are removed every 14 days. The recovery protocol starts the next day and lasts 6 months.
Another technique involves harvesting an autograft from the quadriceps muscle tendon. We also use this technique, being extremely satisfied with the results obtained over the years. The technique involves an incision of about 5 cm in the anterosuperior part of the patella, dissection of the quadriceps tendon, and harvesting of a graft 10 cm long and 7-8 mm wide. The graft will remain inserted by the patella in the upper part, and later it is rotated in the medial area of the patella.
.jpg) |
It is a simple intervention, with hospitalization of 24 hours, lasts on average 40-60 minutes, and is performed with spinal or general anesthesia.
One of the most used techniques, in our practice, is with autograft of large adductor tendon. It is also a minimally invasive technique, which consists of an incision of about 3 cm in the medial area of the knee, the discovery of the tubercle of the large adductor, and the harvesting of a 7cm long graft in adults and 6 cm in children, on the same incision.
Subsequently, another incision of about 2 cm is made on the medial side of the patella, the space between the prepatellar and periosteal bursa is dissected and the graft is fixed with 3 sutures.
.jpg)
Our team's decision to use one of the 3 surgical techniques depends on each case, its complexity, the patient's age, weight, and level of sports activity. In children, we use exclusively the version with large adductor graft, being the least invasive, without bone tunnels and implants.
Regardless of the technique used, hospitalization lasts 24 hours, and recovery lasts on average 6 months. Patients can step on the foot the next day, and use an orthosis for 4 weeks.
Following any surgery, medical recovery plays an essential role in the social, professional, and family reintegration of the patient. Because we pursue the optimal outcome for each patient entering the clinic, recovery medicine from Centrokinetic is based on a team of experienced physicians and physical therapists and standardized medical protocols.

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT


















































































































































