See details
READ MORE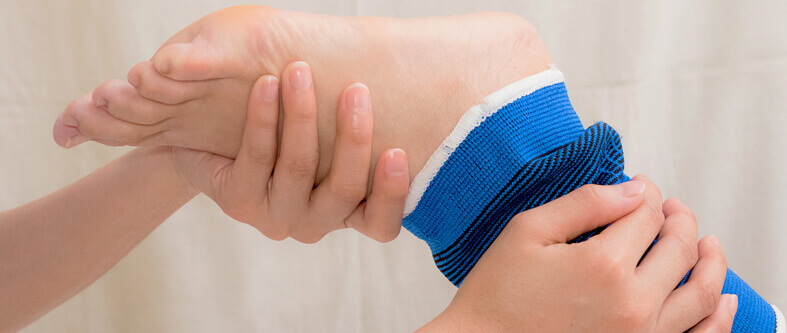
Recovery of the ankle and foot
Even mounts, flat feet, hammer toes and ingrown toenails can be hereditary conditions of the foot. Hormonal changes, age, lifestyle, diet, exercise and other associated conditions contribute to the development of these disease in the foot.
Another very important factor is the race. In the Asian population, bone density is lower than in the white race, and the bone density of the white population is lower than that of the negro race. In the negro race (even if it has a higher risk of suffering from corns, flatulence and calluses), there are 20% fewer diseases of the foot or ankle than in the white race.
The structure of the foot can be influenced by both nationality and geographical origin. For example, the northern Europeans have very high plantar (foot) arches, and the Mediterranean have reduced them. Standards play a very important role in certain ethnic and cultural communities, because their members can use specific, traditional footwear. Strictly enforcing these rules affects many people in the use of various types of shoes.
An important factor in awareness and prevention of foot diseases is the understanding by patients of the role of genetic factors (unchangeable) and those related to lifestyle (often modifiable). In the following, we will inform you about the methods of treatment of the most common diseases of the foot in humans.

Achilles tendon:
There are many conditions in the Achilles tendon that can cause pain in the back of the calf, for example: tendinitis, tendinopathy, tendinosis and tendocalcaneal bursitis. In severe cases, the Achilles tendon can rupture.
Etiology. Achilles tendon disorders can occur in a variety of ways.
- First, there is an irritation of the outer covering of the tendon (paratenon) which causes paratendinitis (an inflammation around the tendon). Inflammation of the tendocalcaneal bursitis may be concomitant with peritendinitis.
These conditions can be caused by the use of improper footwear, intense physical activity or light but repeated physical exertion. Initially, pain and inflammation appear in the tendocalcaneal bursitis. The region reddens, becomes painful, swollen and sensitive to palpation. Achilles tendon pain is specific to Achilles tendonitis. The tendon becomes sensitive to palpation and thickens (ultrasound visible).
A rupture of the Achilles tendonis a significant event because it resembles an extremely strong blow to the calf.
The diagnosis is established with the help of a brief history of the patient and a physical examination. The physical examination identifies the location of the pain and finds, by palpation, where the tendon rupture took place. To confirm the diagnosis, a magnetic resonance imaging (MRI) or an ultrasound can be performed.
Non-surgical treatment. If an inflammatory process is present, the response of the condition to medication and anti-inflammatory intervention should be rapid. Physiokinetotherapy is recommended for any condition of the Achilles tendon. Depending on the type of damage, a personalized treatment will be established.
Surgical treatment is not recommended for most patients. Options can range from a tenotomy (a simple tendon release) to a more complex approach.
Flat foot valgus in adults
By the collapse of the medial longitudinal arch of the foot, a painful condition occurs which is called acquired flatus. The condition is not present from birth or during childhood, but occurs after the end of the growth process. The talo-navicular calcaneal ligament complex is responsible for the formation of the adult flatus, which supports the talonavicular articulation.
The factors involved in flattening deformity in adults are the weakening and damage of the ligaments responsible for supporting this arch.
There are a number of factors that lead to the development of this condition. For example: injuries to the nerves, ligaments or tendons in the foot can all lead to subluxation (partial dislocation) of the subtalar or talonavicular articulation. The fracture is a possible cause. The most common cause is rheumatoid arthritis. Half of the patients with this type of arthritis develop, gradually and progressively, flatus over time.
Initially, pain and inflammation will appear in the medial part of the foot. Progressively, the posterior tibial tendon will sag, rupture, and the pain will intensify. Pain along the side edge of the foot is present in some patients.
The most important steps in establishing the diagnosis are the physical examination and the medical history. X-rays are used to study the position, firmness, alignment of bones, legs and ankles.
Non-surgical treatment is the first recommendation. In some cases, a shoe change may be sufficient. Sometimes, the use of shoes with a good medial arch support or heels is the right solution. Anti-inflammatory drugs may be helpful. People with greater deformity and painful symptoms may benefit from personalized plantar supports. For toning and stretching muscles, a physical therapy program is recommended.
Arthrodesis (fusion), osteotomy (cutting a bone feather), and elongation of the lateral spine (including the use of a bone graft at the calcaneocuboid articulation) are common surgical procedures used in this type of condition. This procedure restores the median longitudinal arch (arch on the inside of the foot).
Shortening, lengthening or transposing tendons are other surgical options. The patient's condition will determine the method of surgical approach.

Taylor’s Bunion(Taylor’s Bunion)
The Taylor’s Bunion is similar to the mount that appears on the race I, but is formed on the outside of the foot, at the level of the fifth toe. The condition got its name because the tailors stood cross-legged for a long time during the day, which led to deformity.
The Taylor’s Bunion has the appearance of an abnormal swelling at the end of the fifth metatarsal (metatarsal head), which rubs against too narrow shoes. The constant pressure leads to the formation of a callus and a thickening of the tissues, which produces a painful mount on the outside of the foot. The thickened tissues underneath become irritated and painful. The reduction of pressure is the only way to reduce pain. Changing narrow shoes can reduce the pressure on the outside or inside.
The symptoms of Taylor's Bunion include: pain, difficulty in wearing shoes and the presence of an unsightly area.
The diagnosis for the Taylor’s Bunion is easily established on the basis of physical examination. X-rays show a possible deformity of the foot and help the doctor decide on the steps in case of need for surgery.
Non-surgical treatment. Using the right shoes (wide enough in front) is the initial treatment. Relieving pressure and reducing pain can also be achieved by applying patches to the mount. The patches are found in pharmacies, are small, have a round shape and a hole in the center.
Surgical treatment. The surgical approach involves removing the mount to release pressure. The fifth metatarsal is also surgically realigned, in case of foot deformity.
When your doctor decides that the intermetatarsal angle is enlarged, the fifth metatarsal bone will be cut and realigned.
Hallux valgus
It is a pathology in which the first metatarsal and the big toe are affected. The condition is usually referred to as mount. By mount, referring to the prominence formed on the medial part of the first metatarsophalangeal articulation. In fact, the condition is much more complex than a simple bump on the medial side of the finger. The shoes wide enough decrease the chances of forming a prominence and help reduce the irritation of the mount, if it is already one.
Most foot problems are due to abnormal pressure or friction. The symptoms appear due to the tightness of the skin and the soft tissues between the hard bone inside, the shoe being hard on the outside. The formation of a callus is the skin's reaction to friction and continuous pressure, and the soft tissues react by thickening. Thick callus and tissue will be irritated and painful. The mount also includes the bone deformity of the metatarsal I and the big toe, the causes can be hereditary, the result of wearing shoes that are inappropriate or of unknown origin. Relieving pressure is one way to reduce pain.
Symptoms focus on the mount, which is painful. For many patients, a severe deformity can be painful and unsightly. Buying the right shoes becomes difficult, especially for women who want to be fashionable. The deformity begins to move upwards, at the level of the second toe, constantly rubbing against the shoe.
The diagnosis begins with the doctor performing a detailed history and a physical examination. This includes: a discussion of the importance of footwear in the development and treatment of the condition. X-rays will be recommended. These will allow the doctor to measure the important angles of the bones in the legs, in order to establish an appropriate treatment.
Non-surgical treatment. The initial treatment in hallux valgus is done by switching to shoes that fit the foot. In the early stages of the mount, switching to appropriate footwear can slow down or stop the deformation process. The treatment is focused on relieving pressure because it causes pain.
Surgical treatment. If non-surgical approaches fail to control symptoms, then surgery is recommended. There are over 100 known surgical procedures for treating mounts. The basic factors considered in performing any surgery are:
- the excision of the mount;
- bone realignment;
- balancing the muscles around the articulation (to prevent recurrences).

Mallet finger / Claw hand
The claw hand and the mallet finger are common pathologies in people who wear inappropriate shoes. The front of the forefoot and the toes are made up of several bones. Each of the four little toes begins with a metatarsal bone in the front of the foot, followed by three other small bones called phalanges.
The first of these small bones is called the proximal phalanx. Then comes the middle phalanx, and the last is the distal phalanx. In a mallet finger deformation, the first articulation is bent upwards, and the middle articulation is downwards. The claw hand has the first articulation curved upwards, and both the middle articulation and the articulation at the tip of the finger are deflected downwards like a claw.
The two causes may be due to wearing inappropriate (small) shoes. It is common for the second toe to be longer than the big toe, and the fit of the shoe tends to fit the first toe, the second toe, and even the third will bend to fit the shoe.
A mallet finger is also a problem for people who have big toe mounts. The claw hands are common in people with high arch. Gradually, the toes, which are crushed daily, will be fixed in this position and will not straighten. In this situation, the pressure appears in three places:
- at the end of the finger;
- at the level of the first articulation;
- at the level of the middle articulation.
The diagnosis of these two pathologies is evident on physical examination. However, it is important to eliminate the presence of neurological conditions that can cause your pathology, especially in the case of the claw hand. Other special tests may be performed.
Non-surgical treatment. The treatment is determined by the severity of the damage. Initially, simply switching to the right type of footwear can stop the deformity, and the toes can return to a better condition.
Surgical treatment. If the non-surgical treatment does not improve the symptoms, surgery is suggested to reposition the toe. In case of deformity of the mallet finger, arthroplasty of the distal articulation is recommended. The most common method of correcting the deformity of the claw hand is arthroplasty of the proximal articulation.
The scar tissue formed by the healing of the articulation will connect the two bones together.
A common procedure is arthrodesis (blocking) of the affected articulation.
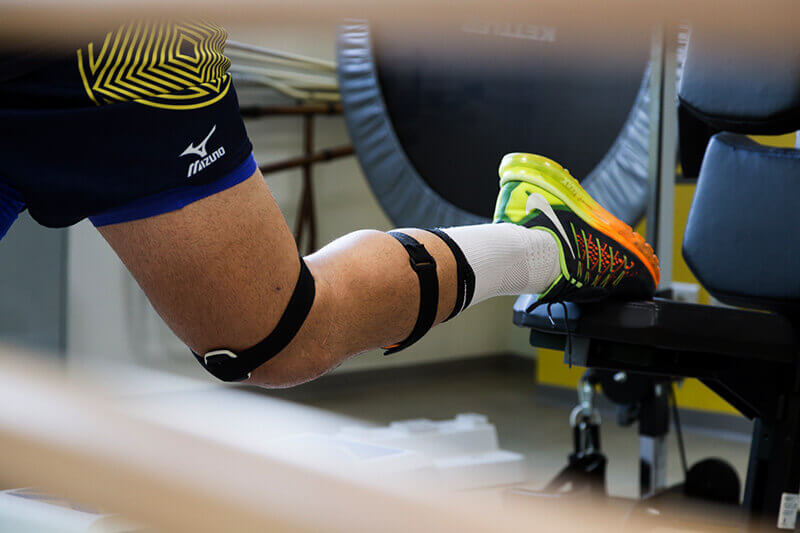
Hallux rigidus
It is a type of degenerative arthritis and affects the metatarsophalangeal articulation at the base of the big toe. There is a process of wear and degeneration if the articular cartilage covering the two bone surfaces is affected. The cause that leads to Hallux Rigidus is not completely discovered, what is known so far, is that the pathology begins with an injury in the area. This issue may remain unknown for a long time. There are cases in which the damage occurs without prior injury, which indicates that there are other causes that can cause Hallux Rigidus.
Following an X-ray that will show the exact extent and location of the disease, a diagnosis will be made.
Non-surgical treatment. It starts with the administration of an anti-inflammatory medication that will relieve pain and prevent finger enlargement. It is recommended to use special footwear and perform an injection on the wrist, which will improve your symptoms.
Surgical treatment. Surgical treatment is used if any other procedure has failed. There are many surgical techniques, indicated depending on the severity of the patient's problem. The operation can be done either to replace the finger articulation or to fuse the affected articulations. Depending on the condition, other surgical methods may be used to replace two wrists.
.png)
Plantar Fasciitis
Represents the painful condition that affects the lower leg. Heel pain is often caused by it. Plantar fasciitis is the name used correctly when active inflammations are encountered. Almost 30% of cases involve both legs. The plantar fasciitis is a thick band of connective tissue. It contributes to the support of the arch of the foot and is located between the heel and the forefoot.
The plantar fasciitis is composed of collagen fibers oriented in a longitudinal direction, starting from the toes to the heels.
Plantar fasciitis can have a number of causes. Identifying the causes of this pain can be difficult. When the foot supports all the weight of the body, it is centered on the plantar fasciitis. This stress leads to the attachment of the fascia to the heel. Small ruptures of the fascia can occur, which can be repaired by the body. The appearance of osteophytes along with the fascia is not the cause of the problem. As the body ages, there is a degeneration and thinning of the fleshy part of the heel. Some doctors believe that the nerves that have passed through the plantar fascia on their way to the front of the foot are irritated and contribute to pain.
Symptoms of plantar fasciitis include pain along the inner edge of the heel, near the arch of the foot. The symptoms are severe when the weight is placed on the leg, especially after a long period of rest or inactivity. The pain is most intense in the morning, when the foot is first placed on the floor. The symptom, also known as first-degree pain, is specific to plantar fasciitis. Standing upright for a long time accentuates the painful symptom. Pulling your toes from back to front can be very painful.
The diagnosis of plantar fasciitis is made following the patient's history and clinical examination. There can be several factors that generate pain, from which the fascia must be differentiated.
Performing special tests helps determine the exact etiology. To eliminate the presence of a heel fracture and to highlight a possible bone spur, an X-ray is performed.
Non-surgical treatment. In most patients, non-surgical treatment is sufficient.
Wearing a splint at night has given some patients positive results, reporting a reduction in pain when leaving the foot on the floor in the morning. Supporting the medial arch with a plantar support helps reduce pressure on the plantar fascia. Once a week, for 3 weeks, the shock wave treatment can be combined. Anti-inflammatory medication is sometimes given to reduce inflammation and to reduce pain. A cortisone injection may also be given into the fascia area.
Surgical treatment. Surgery is a last resort solution for treating heel pain. Several procedures have been developed in the last hundred years to try to treat heel pain:
- excision of the bony spur (if it is present);
- plantar fascia release (plantar fasciotomy);
- releasing pressure on the small nerves in the area.
The operation is done through a small incision on the inner edge of the foot, although now this type of operation can be performed with an endoscope. Surgery involves locating the area where the plantar fascia is inserted on the heel and partially releasing the fascia. If a small spur is present, it will also be removed.
SUCCESSFUL RECOVERY STORIES

MAKE AN APPOINTMENT
CONTACT US
MAKE AN APPOINTMENT
FOR AN EXAMINATION
See here how you can make an appointment and the location of our clinics.
MAKE AN APPOINTMENT















































































































































